To serve the economic and societal demands of our 24/7 society, it is becoming increasingly necessary for employees to work outside the traditional daytime working hours. About 15–20% of employed adults in Europe and the USA currently work in shifts (1, 2). Shift work has, however, been linked with adverse health effects, including metabolic disturbances, such as alterations in body weight, glycaemia and lipids (3–6), and several chronic diseases, such as breast cancer, type 2 diabetes and cardiovascular diseases (6–9).
To alleviate these adverse health effects of shift work, there is a need for insight into the mechanisms that underlie this relationship. The causal mechanisms linking shift work and disease seem to be multifactorial. Lifestyle behaviors, such as poor dietary behaviors, have been hypothesized as one of the contributing factors of the adverse health effects of shift work (8, 10). Several studies have suggested that shift workers have poorer dietary behaviors than day workers (11, 12). During irregular shifts, shift workers tend to eat a larger number of small meals and eat more at irregular times (13, 14). As to their usual diet, shift workers seem to consume more high-energy snacks and sugars than day workers (14–17). Shift workers were also found to have a lower intake of fruits and vegetables (17, 18), fiber (19) and some vitamins and minerals (eg, vitamin B, C, magnesium) (19) than day workers. In contrast, one study has shown a higher consumption of fruits for shift workers in comparison with day workers (20), and other studies showed no differences for fruits and vegetables (21), vitamin C (18) and fiber (18, 22).
As pointed out in Lowden et al’s review, most studies on shift work and diet had insufficient statistical power and used unreliable methods to measure nutrient and food intake (11). Most of these studies also lacked adjustment for major confounders, such as age (13–17, 19–24). Another important drawback is that the available studies focused on single nutrients or foods (13–24). For a comprehensive evaluation of differences in dietary intake, it is important to study dietary patterns because different nutrients and foods have additive and synergistic interactions (25). Overall dietary pattern scores, such as the Mediterranean Diet Score (MDS) or the World Health Organization (WHO)-based Healthy Diet Index (HDI), provide a broad picture of diet quality (25), and higher scores are associated with a lower risk of metabolic disturbances and chronic diseases (26, 27). In addition, a higher energy intake (ie, quantity of food) has also been associated with body weight gain and other metabolic disturbances (20, 28). Therefore, we hypothesized that shift workers have a poorer overall diet quality and higher energy intake than day workers. Dietary patterns may be more altered with a higher frequency of night shifts because night shifts desynchronize circadian rhythms and require the reorganization of food intake due to a changed sleep schedule (29). For that reason, we also hypothesized exposure–response relationships of a higher frequency of night shifts and years of shift work with poorer diet quality and higher energy intake.
Our aim was to compare quantity and quality of the usual diet between day and shift workers and to study exposure–response relationships regarding the frequency of night shifts and number of years of shift work.
Methods
Study population
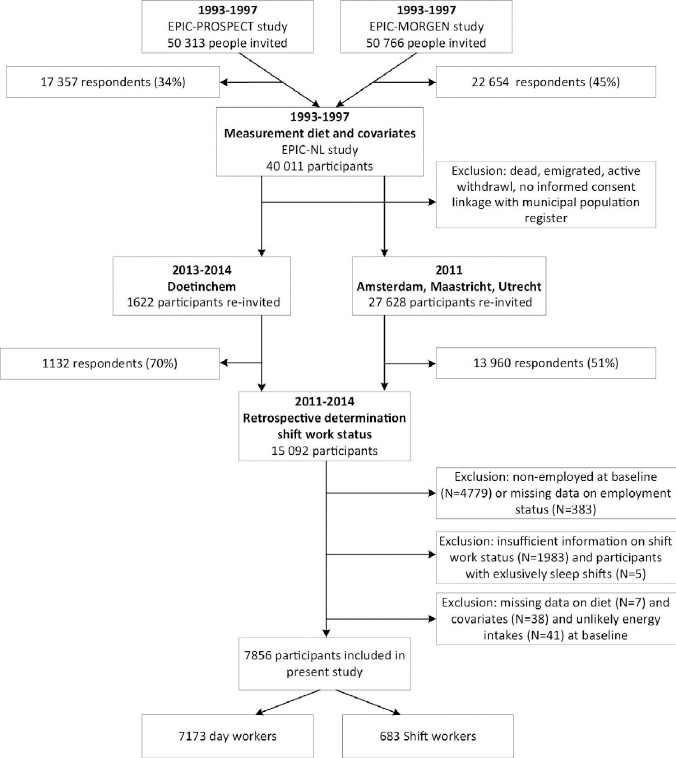
The study comprised data from the Dutch part of the European Prospective Investigation into Cancer and Nutrition (EPIC-NL) that consists of the EPIC-MORGEN and EPIC-PROSPECT cohorts. The EPIC-MORGEN cohort comprises a general population sample of 22 654 men and women (participation rate: 45%) aged 20–65 years in 1993–1997 from three Dutch towns (Amsterdam, Maastricht, and Doetinchem). The EPIC-PROSPECT cohort consists of 17 356 women (participation rate: 35%) aged 49–70 who participated in a breast cancer screening program in Utrecht, the Netherlands. Details of the study design of EPIC-NL have been described elsewhere (30). For the present analyses, participants who also responded to a questionnaire in 2011–2014 (N=15 092) were eligible. This questionnaire included questions on shift work history and enabled us to determine shift work status retrospectively in 1993–1997. We excluded participants without work or missing data on shift work, employment status and covariates, leaving data of 7856 participants for the present analyses (figure 1). All participants gave written informed consent and the Medical Ethics Committees of the University Medical Center Utrecht and the TNO Nutrition and Food Research Institute approved the study.
Shift work
In 2011–2014, participants completed a questionnaire about shift work history based on the most important aspects of shift work as defined in the consensus report of the International Agency for Research on Cancer (IARC) (31). Participants were asked to report whether or not they ever worked in evening, night, sleep and/or rotating shifts. “Evening shift” was defined as a shift that ended before midnight; “night shift” as a shift that continued or started after midnight; “sleep shift” as a shift where people sleep at work and are awakened if necessary; and “rotating shift” as alternation between day, evening, sleep and/or night shifts. If participants responded that they worked in shifts, they were asked to report the following three items for each type of shift work: (i) the year they started shift work; (ii) the year they stopped shift work; and (iii) the number of years and months they worked in shifts. This information was used to determine shift work retrospectively at the time of the dietary measurements (1993–1997). Participants who worked in evening, night or rotating shifts were considered as shift workers, and all others were categorized as day workers.
The number of years participants had worked in shifts before the dietary measurements (1993–1997) was categorized into <10, 10–19, and ≥20 years. Participants who worked in night or rotating shifts (N=614) were also asked the following question: “on average, how many times per month did you work ≥3 hours between midnight and 5 am?” The frequency of night shifts was categorized into no night shifts (ie, exclusively evening shifts or rotating shifts without night work), and 1–4, and ≥5 night shifts/month.
Measures
In 1993–1997, dietary intake was assessed using a validated 178-item semi-quantitative Food Frequency Questionnaire (FFQ) (32, 33). Quality of the diet was operationalized with the modified MDS defined by Trichopoulou et al (34) and the HDI based on the WHO dietary guidelines (35). Based on gender-specific medians of the whole EPIC-NL population, values of 0 or 1 were assigned to nine nutritional components (vegetables, fruits, legumes and nuts, grains, fish and seafood, unsaturated to saturated fatty acid ratio, dairy, meat and alcohol). This led to a score ranging from 1–9, with a higher score indicating a healthier diet. The HDI assigned values of 0 or 1 to six nutrients (ie, saturated fatty acids, polyunsaturated fatty acids, cholesterol, protein, dietary fiber, free sugars) and one food group (ie, fruits and vegetables). A value of 1 was assigned to each component if the intake was within the recommended range according to WHO guidelines (35). All components were summed to form a score ranging from 0–7, with a higher score reflecting a healthier dietary pattern. For more insight into diet quality, we additionally assessed the following four food groups: percent energy derived from soft drinks and fruit juices, sweets (sugar, honey, chocolate, confectionary, ice cream), cake and biscuits, and savory snacks (spring rolls, Russian salad, pizza, Dutch fried meat snacks, French fries).
All covariates were assessed in 1993–1997. Participants completed a questionnaire including questions on demographics (age, gender, education and marital status) and lifestyle (physical activity and smoking). Physical activity was categorized into four categories ranging from inactive to highly active using the validated Cambridge Physical Activity Index (CPAI) (36). The CPAI combines type of work (ie, sedentary or no job, standing, physical or heavy manual job) and the amount of leisure-time physical activity (ie, walking, cycling, gardening, home repair (do-it-yourself), housework, and physical exercise). Physical activity was not measured in this format at the first year of the EPIC-MORGEN study. Missing CPAI scores (15%) were imputed by single linear regression modelling to reduce bias. Body weight was measured to the nearest 0.1 kg and height to the nearest 0.5 cm. Smoking status was categorized as never, former and current smoking (≥1 cigarettes/day). Body mass index (BMI) was calculated as weight divided by height squared, and obesity was defined as a BMI ≥30 kg/m2.
Data analysis
Linear regression analyses with estimation of robust standard errors (SE) were used to assess the associations of shift work with dietary variables; regression coefficients (β) and 95% confidence intervals (95% CI) were obtained. The SE obtained from this method is considered to be more robust and can deal with concerns about failure to meet assumptions that relate to normality and heteroscedasticity (37). Dietary variables were included as dependent variables and shift work (no/yes) was included as independent variable. To study exposure–response relationships regarding frequency of night shifts with dietary patterns, three groups of shift workers (0, 1–4, and ≥5 night shifts times/month) were compared to day workers. Shift workers were also categorized by years of shifts work (<10, 10–19, and ≥20 years) and compared to day workers. All analyses were adjusted for age, gender, educational level, marital status, smoking status and physical activity. Analyses on energy intake were additionally adjusted for BMI to control for variability in energy demands due to differences in BMI between day and shift workers. Possible interaction between shift work and gender was statistically tested using an interaction term between the two. If the interaction term was statistically significant (P<0.05), we conducted analyses for men and women separately. We performed sensitivity analysis to evaluate whether our results were robust to problems with the assumptions of normality and heteroscedasticity. Box-cox power transformations were used to normalize the outcome variables (38), and these transformed outcome variables were included in multivariable-adjusted linear regression models. The results of this sensitivity analysis were similar as the primary analysis but more difficult to interpret and are therefore not presented. All analyses were performed using SAS 9.3 software (SAS Institute, Cary, NC, USA) and a two-sided P-value of <0.05 was considered statistically significant.
Results
The study population consisted of 7173 day workers and 683 shift workers. Of the shift workers, 73% had ≥1 night shift/month and 31% did shift work for ≥20 years. The mean age in 1993–1997 was 47 years (range: 20–70) and 30% of the participants were men. More than a third of the population (36%) had a high level of educational attainment. Compared to day workers, shift workers were less often highly educated, more often smokers and physically active, and had a slightly higher BMI (table 1). Shift workers had a higher median energy intake than day workers (2222 kcal/d versus 1990 kcal/d) but the same median MDS (5) and HDI (3).
Table 1
Characteristics (1993–1997) of day and shift workers. [SD=standard deviation; IQR=interquartile range; BMI=body mass index; MDS=Mediterranean diet score; HDI=healthy diet indicator.]
| Day workers (N=7173) | Shift workers (N=683) | |||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|||||||||||
| N | % | Mean | SD | Median | IQR | N | % | Mean | SD | Median | IQR | |
| Demographics | ||||||||||||
| Age (years) | 47.0 | 10.6 | 42.7 | 10.1 | ||||||||
| Gender (male) | 2019 | 28 | 312 | 46 | ||||||||
| High educational level (higher vocational education or university) | 2666 | 37 | 177 | 26 | ||||||||
| Marital status (married, living together) | 4983 | 69 | 441 | 65 | ||||||||
| Occupational | ||||||||||||
| Number night shifts per month | 232 | 34 | 4 | 1–7 | ||||||||
| Years of shift work | 237 | 35 | ||||||||||
| <10 | 214 | 31 | ||||||||||
| 10–19 | ||||||||||||
| ≥20 | ||||||||||||
| Lifestyle | ||||||||||||
| Current smoker | 1783 | 25 | 223 | 33 | ||||||||
| High physical activity level a | 3346 | 47 | 421 | 62 | ||||||||
| BMI (kg/m2) | 24.8 | 3.5 | 25.4 | 4.0 | ||||||||
| Overweight (BMI 25–30 kg/m2) | 2552 | 36 | 265 | 39 | ||||||||
| Obesity (BMI ≥30 kg/m2) | 645 | 9 | 69 | 10 | ||||||||
| Waist circumference (cm) | 83 | 11 | 85 | 12 | ||||||||
| Diet | ||||||||||||
| Total energy intake (kcal/d) | 1990 | 1670–2391 | 2222 | 1826–2700 | ||||||||
| Percent energy from fat | 35.4 | 32.1–38.6 | 35.6 | 32.6–38.6 | ||||||||
| Percent energy from carbohydrate | 44.9 | 41.0–49.0 | 45.4 | 41.2–49.0 | ||||||||
| Percent energy from protein | 15.9 | 14.5–17.5 | 15.8 | 14.4–17.3 | ||||||||
| MDS (score 0–9) | 5 | 4–6 | 5 | 4–6 | ||||||||
| Cereals and grains (g/d) | 49 | 26–77 | 58 | 34–96 | ||||||||
| Fruits (g/d) | 245 | 144–357 | 221 | 126–330 | ||||||||
| Vegetables (g/d) | 130 | 102–167 | 130 | 100–165 | ||||||||
| Legumes and nuts (g/d) | 34 | 22–48 | 35 | 22–50 | ||||||||
| Fish and seafood (g/d) | 8.0 | 3.3–14.9 | 8.2 | 3.7–14.8 | ||||||||
| Meat and meat products (g/d) | 102 | 62–136 | 118 | 78–159 | ||||||||
| Dairy products (g/d) | 346 | 197–541 | 358 | 181–580 | ||||||||
| Fatty acid ratio | 1.38 | 1.22–1.55 | 1.41 | 1.27–1.57 | ||||||||
| Alcohol (g/d) | 8.2 | 2.0–19.3 | 7.5 | 1.9–19.8 | ||||||||
| HDI (score 0–7) | 3 | 3–4 | 3 | 3–4 | ||||||||
| Percent energy from saturated fat | 14.6 | 12.8–16.0 | 14.2 | 12.8–15.7 | ||||||||
| Percent energy from polyunsaturated fat | 6.5 | 5.5–7.7 | 6.7 | 5.7–7.7 | ||||||||
| Cholesterol (mg/d) | 211 | 167–261 | 232 | 184–287 | ||||||||
| Percent energy from protein | See above | See above | ||||||||||
| Dietary fiber (g/d) | 23 | 20–28 | 25 | 20–30 | ||||||||
| Fruits and vegetables (g/d) | 379 | 273–504 | 356 | 249–483 | ||||||||
| Percent energy from free sugars | 5.8 | 3.7–8.6 | 5.8 | 3.3–8.9 | ||||||||
| Savory snacks (g/d) | 23 | 6–59 | 45 | 15–77 | ||||||||
| Sweets (g/d) | 29 | 15–51 | 33 | 15–59 | ||||||||
| Cake and biscuits (g/d) | 25 | 13–41 | 23 | 11–40 | ||||||||
| Soft drinks and fruit juices (g/d) | 131 | 57–220 | 161 | 84–272 | ||||||||
Shift work and macronutrient intake
Results of the multivariable-adjusted analyses showed that shift workers had a statistically significantly higher usual energy intake than day workers: they consumed 56 kcal/d (95% CI 10–101) more than day workers (table 2). The percentage of energy derived from protein was slightly higher among shift compared to day workers (β: 0.29%, 95% CI 0.11–0.46). No statistically significant differences were observed for the percent energy from carbohydrates (β: -0.34%, 95% CI -0.80–0.11). Among women, the percent energy from fat was higher among shift than day workers (β: 0.67%, 95% CI 0.16–1.17); among men, there was no significant difference between groups (β: -0.14%, 95% CI -0.70–0.43) (P=0.04 for the interaction between shift work and gender).
Table 2
Differences a between day and shift workers in the Mediterranean diet score (MDS), healthy diet indicator (HDI) and their components. [95% CI=95% confidence interval]. Significant associations (at P<0.05) are printed in bold.
a Presented as regression coefficients (95% confidence intervals) of the difference in the mean levels of diet components between day and shift workers obtained by linear regression with robust standard errors adjusted for age, gender, education, marital status, smoking status and physical activity. Energy intake was additionally adjusted for body mass index.
Shift work and quality of diet
No statistically significant differences in MDS (β: 0.1, 95% CI -0.0–0.5) and HDI (β: 0.0, 95% CI -0.1–0.1) were observed between day and shift workers (table 2), ie, the overall quality of diet was similar in both groups. However, there were statistically significant differences between groups in some of the components of the MDS and HDI. Among shift workers, usual intake of cereals and grains was 8 g/d (95% CI 3–12), fish and seafood 0.9 g/d (95% CI 0.1–1.8), meat 6 g/d (95% CI 2–10), dairy products 31 g/d (95% CI 6–56) and cholesterol 10 mg/d (95% CI 4–17) higher than day workers. The usual percentage energy derived from cake and biscuits was lower among shift than day workers, and that of savory snacks, sweets, and soft drinks and fruit juices was similar (P>0.05). The interaction term between shift work and gender was significant for savory snacks (P=0.03), but shift work was not associated with savory snacks among both men (β: -0.3%, 95% CI -0.8–0.2) and women (β: 0.1, 95% CI -0.3–0.5).
Night shift frequency, shift work years & dietary patterns
Compared to day workers, shift workers with ≥5 night shifts per month had a 1.4 kg/m2 higher BMI, a 5 cm larger waist circumference, and were more often obese (16% versus 9%). In contrast, participants without night shifts (eg, exclusively evening shifts) and those with 1–4 night shifts/month had a similar BMI and waist circumference as day workers (data not shown). After adjustment for the differences in BMI, total energy intake was not statistically significantly higher among shift workers without night shifts (β: 71 kcal/d, 95% CI -14–155) and statistically significantly higher in shift workers with ≥5 night shifts/month (β: 103 kcal/d, 95% CI 29–176) compared to day workers (table 3). Energy intake was not higher among those with 1–4 night shifts/month (P>0.05). No exposure–response relationships were observed between number of years of shift work and usual dietary patterns (Table 4).
Table 3
Differences a in the Mediterranean diet score (MDS), healthy diet indicator (HDI) and their components in shift workers according to number of night shifts compared to day workers (reference category). [95% CI=95% confidence interval]. Significant associations (at P<0.05) are printed in bold.
| Shift workers without night shifts (N=168 b) | 1–4 night shifts/month (N=190 b) | ≥5 night shifts/month (N=264 b) | P-value for trend | ||||
|---|---|---|---|---|---|---|---|
|
|
|
|
|||||
| ß | 95% CI | ß | 95% CI | ß | 95% CI | ||
| Total energy intake (kcal/d) | 71 | -14–155 | -27 | -110–57 | 103 | 29–176 | 0.02 |
| Percent energy from fat | 0.43 | -0.27–1.13 | -0.39 | -0.30–1.08 | 0.09 | -0.51–0.68 | 0.33 |
| Percent energy from carbohydrate | -0.30 | -1.18–0.58 | -0.60 | -1.41–0.21 | 0.16 | -0.54–0.85 | 0.67 |
| Percent energy from protein | 0.25 | -0.10–0.60 | 0.25 | -0.03–0.54 | 0.21 | -0.07–0.49 | 0.02 |
| MDS (score 0–9) | 0.03 | -0.22–0.27 | 0.15 | -0.07–0.37 | 0.10 | -0.09–0.28 | 0.13 |
| Cereals and grains (g/d) | 9 | 1–17 | 8 | 1–16 | 8 | -0–15 | <0.01 |
| Fruits (g/d) | -14 | -36–8.4 | -3 | -27–20 | -1 | -19–17 | 0.68 |
| Vegetables (g/d) | 4 | -4–11 | 2 | -5–10 | 5 | -2–12 | 0.09 |
| Legumes and nuts (g/d) | 2.5 | -1.2–6.3 | 1.1 | -2.7–4.9 | 0.0 | -2.9–2.9 | 0.58 |
| Fish and seafood (g/d) | 1.3 | -0.6–3.1 | 0.5 | -0.8–1.9 | 0.8 | -0.6–2.1 | 0.12 |
| Meat and meat products (g/d) | 5 | -2–12 | -4 | -11–3 | 12 | 4–19 | 0.01 |
| Dairy products (g/d) | 49 | 1–97 | 12 | -31–54 | 36 | -4–76 | 0.03 |
| Fatty acid ratio | -0.03 | -0.07–0.01 | 0.04 | -0.0–0.01 | 0.02 | -0.01–0.04 | 0.13 |
| Alcohol (g/d) | -1.0 | -3.1–1.1 | 0.4 | -1.9–2.8 | -1.3 | -3.2–0.6 | 0.27 |
| HDI (score 0–7) | -0.13 | -0.30–0.04 | 0.10 | -0.06–0.25 | 0.07 | -0.06–0.21 | 0.25 |
| Percent energy from saturated fat | 0.2 | -0.1–0.6 | -0.1 | -0.4–0.2 | -0.2 | -0.4–0.1 | 0.36 |
| Percent energy from polyunsaturated fat | -0.1 | -0.4–0.1 | 0.3 | 0.1–0.5 | 0.1 | -0.1–0.3 | 0.10 |
| Cholesterol (mg/d) | 14 | 3–26 | -3 | -14–7 | 15 | 5–26 | <0.01 |
| Percent energy from protein | See above | See above | See above | ||||
| Dietary fiber (g/d) | -0.2 | -1.2–0.7 | -0.2 | -1.2–0.8 | 1.1 | 0.1–2.0 | 0.09 |
| Fruits and vegetables (g/d) | -10 | -34–14 | -1 | -27–25 | 5 | -17–27 | 0.85 |
| Percent energy from free sugars | 0.1 | -0.5–0.8 | -0.8 | -1.3–-0.2 | -0.1 | -0.7–0.5 | 0.18 |
| Percent energy from savory snacks | -0.2 | -0.9–0.5 | -0.3 | -0.8–0.3 | 0.2 | -0.3–0.7 | 0.90 |
| Percent energy from sweets | 0.1 | -0.6–0.9 | -0.9 | -1.5–-0.3 | 0.1 | -0.6–0.8 | 0.43 |
| Percent energy from cake and biscuits | -0.1 | -0.6–0.4 | -0.5 | -1.0–-0.03 | -0.2 | -0.7–0.2 | 0.06 |
| Percent energy from soft drinks & fruit juices | 0.3 | -0.2–0.7 | 0.3 | -0.1–0.7 | 0.1 | -0.2–0.4 | 0.12 |
a Presented as regression coefficients (95% confidence interval) of the difference in the mean levels of diet components obtained by linear regression with robust standard errors adjusted for age, gender, education, marital status, smoking status and physical activity. Total energy intake was additionally adjusted for body mass index.
Table 4
Differences a in the Mediterranean diet score (MDS), healthy diet indicator (HDI) and their components according to years of shift work compared to day workers (reference category). [95% CI=95% confidence interval.] Significant associations (at P<0.05) are printed in bold.
a Presented as regression coefficients (95% confidence intervals) of the difference in the mean levels of diet components obtained by linear regression with robust standard errors adjusted for age, gender, education, marital status, smoking status and physical activity. Total energy intake was additionally adjusted for body mass index.
Discussion
We observed that shift workers ate on average 56 kcal/d more than day workers based on reporting of their usual dietary patterns. This seemed to be due to a significantly higher consumption of cereals and grains, meat, dairy products, fish and seafood. A higher energy intake was observed in particular among shift workers with ≥5 night shifts per month, while years of shift work was not associated with energy intake. No differences in MDS, HDI and other measures of diet quality were observed between day and shift workers, regardless of frequency of night shifts and number of years of shift work.
In line with the present findings, one other study observed a significantly higher energy intake in shift workers (22). In contrast to our finding of a higher energy intake among shift compared to day workers, the majority of previous studies observed no significant differences (15, 17, 19, 24, 39, 40). However, three of these studies observed a statistically non-significantly higher energy intake among shift compared to day workers (24,39,40). It is important to note that the quality of these studies was insufficient to make proper inferences about differences in energy intake between groups since these studies had a small sample size (N=25–396) (19, 24, 39, 40) and/or did not adjust for potential confounders such as age, gender and socioeconomic status (15, 17, 19, 24, 39, 40). In addition, we observed that BMI and waist circumference were only slightly higher among shift compared to day workers, suggesting that energy balance was not strikingly different. Yet, shift workers with ≥5 night shifts/month, who had a particularly high energy intake, also had a substantially higher BMI (1.4 kg/m2), waist circumference (5 cm) and were almost two times more often obese than day workers. This indicates that particularly shift workers with a high frequency of night shifts (ie, ≥5 night shifts/month) have a less favorable energy balance than day workers. The aforementioned studies did not take frequency of night shifts into account and observed a relatively small difference in BMI (0.4–0.9 kg/m2) between day and shift workers (15, 17, 24, 39, 40). These studies may consequently not have observed differences in energy intake due to a low average frequency of night shifts.
There may be several reasons for the higher energy intake among shift compared to day workers in our study. First, residual confounding by socioeconomic status may be present since adjusting the analyses for educational level might not be sufficient in this study population. However, sensitivity analysis in which we excluded low and intermediate educated participants gave similar results as those presented (data not shown). In part of the population (69%), we were able to determine occupational sector in 1993–1997. We also re-conducted the analyses in white collar workers only, which also revealed similar results (data not shown). Hence, residual confounding by socio-economic status is unlikely to have contributed greatly to the observed differences in energy intake between day and shift workers. Second, higher energy requirements among shift compared to day workers may have led to a higher energy intake among the former without there being a higher risk of adverse health effects. Although metabolism at rest accounts for the largest part of a person’s energy demand, body size and physical activity are the main determinants of variability in energy intake (41). Physical activity at work may for instance be important because it can be expected that, compared to day workers, shift workers more often have physically demanding jobs. We endeavored to take body size and physical activity into account by adjusting the analyses for BMI and a validated physical activity index (36). This index covers occupational and leisure-time physical activity and was shown to have a high repeatability and strong positive associations with objective measures of the ratio of daytime energy expenditure to resting metabolic rate and cardiorespiratory fitness (36). There is no reason to think that misclassification differs systematically between shift and day workers. In addition, additional analyses with adjustment for occupational physical activity and leisure-time physical activity separately (data not shown) showed similar results. Furthermore, we performed sensitivity analyses among white-collar workers only to limit differences in work-related physical activity between day and shift workers. Still, some residual confounding may exist as we used a broad measurement of physical activity (ie, four categories), and BMI does not capture all aspects of body composition related to energy demands. Finally, another likely reason for the higher energy intake among shift workers is that the shift workers’ shift schedule increased the amount of food intake. If this is the case, then a higher energy intake among shift workers may be one of the causes of shift work-induced overweight, obesity and other adverse health effects. However, future studies should confirm that shift workers, independent of energy demands, indeed have a higher energy intake than day workers.
As to the overall quality of diet, we observed no consistent patterns confirming our hypothesis that shift workers have a poorer diet quality than day workers. Although previous studies often suggested poorer diet quality among shift compared to day workers, each study observed a less healthy consumption of different nutrients or foods among shift workers (13–20, 22–24). In contrast to a less healthy consumption of some food items, it has also been observed that shift workers had a more healthy consumption of nutrients and foods, such as more fruits and less saturated fats, than day workers (13, 18, 20, 22). In our study, shift workers also had both a more healthy (ie, cereals, dairy products and fish) and less healthy (ie, meat and cholesterol) consumption of some nutrients and foods compared to day workers. Inconsistencies across studies may be caused by differences in culture-related dietary habits, occupation, type of shift work and frequency of shifts, which may have resulted in a different effect of shift work on dietary patterns. Overall, shift workers may select different foods than day workers, which differs from one population to the other. Still, the overall quality of diet (average of working and non-working days) may usually be similar among day and shift workers, and an overall poorer diet quality among shift workers may therefore not be one of the causes of shift work-induced adverse health outcomes.
A strength of the present study is that we used a much larger sample of day and shift workers than previous studies (11, 12). In contrast to other studies (11, 12), we were also able to investigate differences between men and women, and associations of frequency of night shifts and years of shift work with dietary patterns. While interpreting the results, some limitations should be taken into account. As discussed above, residual confounding by socioeconomic status and physical activity may have contributed to the observed differences in energy intake between day and shift workers. Shift work was assessed 12–19 years after collection of dietary data. This retrospective measurement of the exposure makes our results vulnerable to information bias. However, this risk is likely to be limited, since performing shift work has a major impact on someone’s life and is relatively easy to remember. Furthermore, dietary intake was assessed using self-reports, which is prone to bias and measurement error. This may have led to non-differential misclassification in our study. In addition, the FFQ provides information on the average food intake over a year. Some shift workers with a low frequency of shifts outside daytime working hours may have reported usual intake of days with regular daytime working hours. These two issues related to the measurement of diet may have led to some underestimation of the differences between shift and day workers. Furthermore, respondents to cohort studies are usually slightly healthier and higher educated than non-responders (42). Individuals who were excluded were also less healthy, had a higher energy intake and a lower educational level than the included individuals (data not shown). Since shift work is more common among adults of lower socioeconomic status, exclusion has likely led to an underestimation of the observed differences in dietary patterns between day and shift workers.
This study showed that shift workers, in particular those with many night shifts, had a higher energy intake than day workers but a similar overall quality of diet. These findings suggest that a higher energy intake among shift workers may be one of the causes of shift work-induced overweight, obesity, and other adverse health outcomes. To draw a sound conclusion on this point, future studies need to confirm that shift workers indeed have a higher energy intake than day workers independent of energy requirements. To obtain more insight in the role of energy intake in the relation between shift work and adverse health outcomes, future research should also elucidate the extent to which energy intake is in the causal pathway between shift work and adverse health outcomes.