Work in the agricultural industry is associated with working long hours, economic difficulties, and uncertainties inherent to farming that might influence mental health. However, the evidence for whether the mental health of farmers differs from that of the general population is scarce and shows mixed results (1). Some studies have found that farmers had lower or similar prevalences of mental health problems compared to the general population or other rural residents (2–4), but two large population-based Norwegian studies found indications that farmers had the highest prevalence of depressive symptoms of all the occupational groups included in those studies (5, 6).
The structural changes in agriculture in recent decades may be another source of stress for farmers in industrialized countries (7). The development has been characterized by new technologies and increasing productivity demands, a decrease in the number of farmers, and an increase in farm size (8). Agriculture in Norway has followed this international trend, and this is reflected in the decrease in the number of Norwegian farms, which was 66% in 1979–2014 and 42% in 1999–2014 (9). Anticipation of job loss can affect a person’s health even before the change in their employment status occurs (10), and it is conceivable that working in an industry under stress has had a negative effect on the mental health of farmers. Studies of farmers’ mental may provide better knowledge of how psychosocial and economic conditions in the labor market in general may affect mental health.
Confounding, particularly due to socioeconomic status or other familial environmental factors, could have contributed to the conflicting results of studies of mental health and farming. It is difficult to control adequately for such possible confounding effects, as they may represent subtle influences during childhood and adolescence that are not easily assessed and recorded in survey data. One way to overcome this limitation is to compare siblings in the same family. When comparing mental health symptom load in relation to different occupations, a family design will control for all confounding from shared factors between the siblings (11). Further, the available literature on the mental health of farmers is largely based on cross-sectional data (1), and there is a need for prospective studies.
We studied the association between occupation at baseline and symptoms of mental distress 11 years later. For better control over unmeasured confounding, we also studied the mental health of farmers compared with their siblings working in other occupations.
Methods
We included participants from all three waves of the Nord-Trøndelag Health Study (Helseundersøkelsen i Nord-Trøndelag, HUNT) in our study. Nord-Trøndelag County is situated in Central Norway and is largely rural. The largest of six major towns has only 21 000 inhabitants (12), and the county has a substantial agricultural production. In all three waves of the HUNT study, all residents of Nord-Trøndelag County aged ≥20 years were invited to participate, including 19-year-olds who would turn 20 in the year of the survey. The participation rate was 89.4% (N=77 205) in HUNT1 (1984–1986), 69.5% (N=65 232) in HUNT2 (1995–1997), and 54.1% (N=50 805) in HUNT3 (2006–2008). Data on participants were gathered in a series of self-report questionnaires and clinical measurements in all three HUNT surveys (13). The total number of participants in all three waves was 106 435.
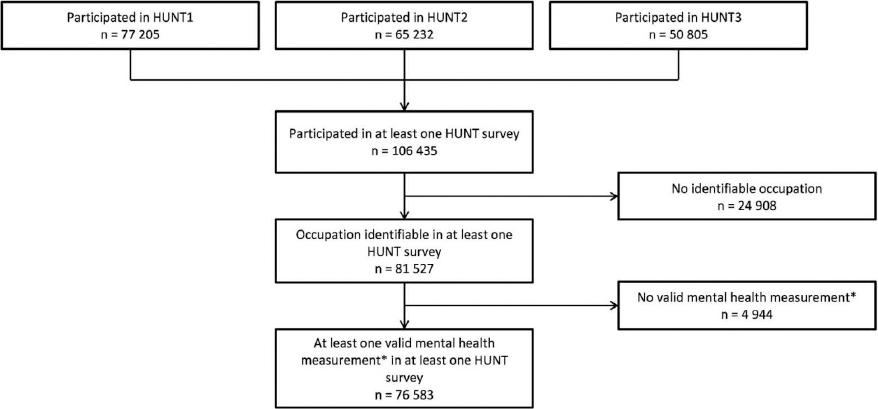
The study population for our study comprised residents of Nord-Trøndelag County who had: (i) taken part in at least one of the three HUNT studies, (ii) had a known occupation (at least one time point), and (iii) had a valid measure of mental health (at least one time point). The selection of participants is shown in figure 1.
Figure 1
The selection of study participants. HUNT = Health Survey of Nord-Trøndelag. HUNT1=first wave (1984–1986). HUNT2= second wave (1995–1997). HUNT3=third wave (2006–2008). *Definitions of valid mental health measurements: HUNT1 and HUNT2 answered all four questions of the Anxiety and Depression Index (ADI). HUNT2 and HUNT3, answered at least five out the seven questions on either the anxiety or the depression subscale of the Hospital Anxiety and Depression Scale (HADS).
Measurement of occupation
Self-reported occupation was measured in different ways in HUNT1, HUNT2 and HUNT3. A comparison of the occupational categories used in the three HUNT surveys is shown in supplementary table 1 (www.sjweh.fi/index.php?page=data-repository). In HUNT1 and HUNT2, participants indicated in which of the nine (HUNT1) or ten (HUNT2) occupational categories they currently worked in, or the last occupation they had worked in if they were not occupationally active at the time of study participation. Being occupationally active at the time of participation in the HUNT study was not a requirement.
Table 1
Overview of and selection of study participants for the prospective cohort analyses. The Nord-Trøndelag Health Study (HUNT). HUNT1 (1984–1986), HUNT2 (1995–1997) and HUNT3 (2006–2008) [ADI=Anxiety and Depression Index; HADS=Hospital Anxiety and Depression Scale]
| Outcome | Symptoms of psychological distress | Symptoms of anxiety | Symptoms of depression |
|---|---|---|---|
| Baseline | HUNT1 | HUNT2 | HUNT2 |
| Outcome measurement | HUNT2 | HUNT3 | HUNT3 |
| Measurement instrument of mental health | ADI | HADS a | HADS b |
| Number who participated in the HUNT study at both time points | 40 802 | 36 229 | 36 229 |
| Excluded | |||
| No mental health measurement at both time points | 15 881 | 6503 | 6260 |
| No occupational measurement at baseline | 1914 | 6421 | 6569 |
| Had outcome at baseline | 2769 | 3350 | 2073 |
| Final study population | 20 238 | 19955 | 21 327 |
The main part of all three study waves of HUNT consisted of two questionnaires given to all participants. Questionnaire 1 (Q1) was sent by mail along with the invitation letter to all residents of Nord-Trøndelag County. Questionnaire 2 (Q2) was handed out at the time of participation and was to be completed at home and returned in a prepaid envelope (14, 15). This resulted in a lower response rate on questions that were in Q2 compared to questions in Q1. The questions on occupation were in Q2 in both HUNT1 and HUNT2. In HUNT3, participants were asked their main occupation in an interview at the health examination sites. Their job title was later classified manually according to the Statistics Norway classification scheme (Standard Classification of Occupations) (16). This classification is based on ISCO-88(COM), which is the European Union version of the International Standard Classification of Occupations (ISCO-88) (17).
In HUNT1 and HUNT3, only the main occupation was recorded for each participant. In HUNT2, a participant could state having two or more occupations. For the purpose of this paper, we assigned one occupation to each participant. We assumed that if a participant had several occupations, the one with the highest socioeconomic status would exert the main influence on the participant’s health. Therefore, we assigned the occupation with the presumed highest socioeconomic status to the participant. The method used for determining socioeconomic status in HUNT2 has been described previously (18).
We classified participants into seven groups using a simplified version of the Erikson-Goldthorpe-Portocarero (EGP) social class scheme (19): (i) higher grade professionals and managers, (ii) lower grade professionals, (iii) routine non-manual workers, (iv) farmers and forest owners/forestry workers, (v) other self-employed, (vi) skilled manual workers, and (vii) unskilled manual workers. Details on the classification are shown in supplementary table 1. For simplicity, hereafter, we refer to the “farmers and forest owners/forestry workers” group as “farmers,” and “higher grade professionals and managers” as “higher grade professionals.” Norwegian farmers are largely self-employed, and own their own land. We therefore called the group of self-employed working in other occupations “other self-employed.” In HUNT3, we included forestry workers in the farmers group because forest owners and farmers were in the same occupational category in HUNT1 and HUNT2. The proportion of forest owners in HUNT1 and HUNT2 is unknown, but the low proportion of forestry workers in HUNT3 (4%) suggests that the majority of those in the combined “farmers and forest owners/forestry workers” group were farmers in all three surveys. When going through the HUNT3 occupational titles manually, we found that a number of agricultural workers had been classified as farmers. Because we wanted our “farmers” group to consist of self-employed farmers working on their own farm, we recoded agricultural workers to the unskilled manual workers group.
Having a health problem may cause downward social mobility, a process known as social drift (20). To reduce bias due to reverse causation, we used an approach similar to the intention-to-treat principle in randomized controlled trials in the sibling study. We used the first available measurement of occupation for each participant, irrespective of any later occupation measurements. In total, there were 24 908 participants with no recorded occupation, and they were excluded from our study.
Measurement of mental health
Different measurement instruments of mental health were used in the three HUNT surveys. In HUNT2 and HUNT3, we used the validated Hospital Anxiety and Depression Scale (HADS) to measure symptoms of anxiety and depression. The HADS consists of 14 symptom questions – 7 related to symptoms of anxiety (HADS-A), and 7 related to symptoms of depression (HADS-D). Each question is rated on a scale of 0–3, yielding two subscales ranging from 0–21, with the maximum score indicating the highest level of anxiety or depression symptoms (21). We defined a valid score as one in which ≥5 of 7 questions on ≥1 subscale had been answered. If a participant had answered 5 or 6 questions on a subscale, the participant’s subscale score was multiplied by 7/5 or 7/6, respectively. A score of 8 has been found the optimal cut-off for both anxiety and depression, with a sensitivity and specificity of ca. 0.80 on both subscales (22). We used a score of ≥8 to define caseness for both anxiety and depression, indicating a possible and probable case of anxiety or depression.
In HUNT1 and HUNT2, we used the Anxiety and Depression Index (ADI) to measure psychological distress. The ADI is a compound measure of four variables concerning nervousness, calmness, mood and vitality. The ADI does not separate anxiety from depression, but has been found to be an acceptable indicator of anxiety and depression symptom caseness. When validated against the HADS, the ADI had a sensitivity of 0.51 and a specificity of 0.93 (23). All four questions needed to be answered in order to secure a valid ADI score. We rescaled all four variables from 0–1, with 0 indicating the lowest symptom level and 1 the highest symptom level. We summed the rescaled variables and divided the sum by four to get a measure between 0 and 1. We defined being in the top decile of the ADI as having a high level of psychological distress, and the cut-off was 0.5.
A total of 4944 participants did not have a valid measure of mental health (ADI or ≥1 HADS subscale) in any of the surveys, and they were excluded. Thus, the size of our study population was 76 583.
Confounding
We used Directed Acyclic Graphs (DAG) to evaluate possible confounding (24). We considered age and sex to be confounders and adjusted for them in the analyses.
Occupation and education are both ways of measuring socioeconomic status (20), and consequently we did not adjust for education in the comparison between farmers and other occupational groups. When comparing farmers with their siblings, education and birth order could have been confounders, and we therefore adjusted for them in the analyses.
Prospective cohort analysis
To investigate the association between occupation at baseline and symptoms of psychological distress, anxiety, and depression, we identified three cohorts that had valid answers on the same mental health symptom scale at two time points (either 1984–1986 and 1995–1997 or 1995–1997 and 2006–2008). The basis for the selection of study participants was everyone in our study material who had participated in both HUNT1 and HUNT2 (for the outcome psychological distress), and HUNT2 and HUNT3 (for the outcomes symptoms of anxiety and symptoms of depression). We excluded study participants who did not have a valid answer on the measure of mental distress in question at both time points. Further, we excluded study participants who did not have an occupational measurement at baseline. Finally, we also excluded study participants who had the outcome in question at baseline. The number of study participants, we well as the number of people who were excluded for each reason in each of the three cohorts, are shown in table 1.
We used logistic regression to investigate the association between occupation at baseline (1984–1986 for symptoms of psychological distress, 1995–1997 for symptoms of anxiety and depression) and having the outcomes 11 years later (the top decile of the ADI, symptoms of anxiety or depression caseness). A total of 1862 study participants (9.2%) had symptoms of psychological distress in 1995–1997, 1544 study participants (7.7%) had symptoms of anxiety caseness in 2006–2008, and 1319 study participants (6.2%) had symptoms of depression caseness in 2006–2008.
We tested for interactions between sex and occupational group in all three cohorts. For symptoms of psychological distress, we found evidence of an interaction between sex and occupational group – the P-value of the likelihood-ratio (LR) test was 0.05 - and therefore the analyses were stratified by sex. For the other two outcomes, we did not find evidence of an interaction (the LR-test P-value was 0.59 for symptoms of anxiety caseness and 0.25 for symptoms of depression caseness), and adjusted for sex. We adjusted for age as a continuous variable in the analyses of symptoms of psychological distress and depression. However, for symptoms of anxiety, there were indications that the relation was not linear, and we adjusted for age as a categorical variable with four categories.
Sibling study
We used fixed effects logistic models to compare farmers with their siblings working in other occupations. We identified siblings using data on ancestry from the National Registry. Ancestry data were linked to HUNT data using the 11-digit unique national identification number, which is given to every resident in Norway at birth or immigration. We defined siblings as persons having the same mother, irrespective of their paternity. Analyses were performed separately for HUNT1, HUNT2, and HUNT3, with psychological distress and symptoms of anxiety and depression caseness as dichotomous outcomes. We adjusted for sex and age as a continuous variable. We linked HUNT data with registry data on education from the Norwegian Education Database (Nasjonal utdanningsdatabase, NUDB), to find the highest level of education achieved by 2012. We adjusted for education level using the following categorical variables: (i) not graduated from secondary school, (ii) secondary school graduate, and (iii) college/university graduate. We also adjusted for birth order as a categorical variable. The participants were classified as their mother’s first, second, third, or fourth or later child.
We tested for interaction between sex and occupation among farmers and their siblings. The interaction terms were not statistically significant for symptoms of psychological distress [HUNT1 (P=0.91), HUNT2 (P=0.25)], anxiety caseness [HUNT2 (P=0.64), HUNT3 (P=0.49)] or depression caseness [HUNT2 (P=0.97), HUNT3 (P=0.29)].
Sensitivity analyses
To increase the probability that siblings had actually grown up together, we performed sensitivity analyses in which we included full siblings only. In the total study material, the identity of both parents was known for 51 829 study participants. Of these, 847 (1.6%) had at least one half-sibling, and were excluded. We also performed sensitivity analyses that included siblings from families with children with a maximum age difference of 10 years only. We used Stata 13.1 (StataCorp, College Station, TX) to perform the analyses.
Results
The characteristics of the study participants in HUNT1, HUNT2 and HUNT3 are shown in table 2. The mean age increased by almost ten years between HUNT1 and HUNT3; the educational level also increased. The proportion of farmers and unskilled manual workers decreased, whereas the proportion of higher and lower grade professionals and routine non-manual workers increased.
Table 2
Characteristics of the study participants. The Nord-Trøndelag Health Study (HUNT). HUNT1 (1984–1986), HUNT2 (1995–1997) and HUNT3 (2006–2008) [SD=standard deviation; HADS=Hospital Anxiety and Depression Scale]
| HUNT1 | HUNT2 | HUNT3 | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
||||||||||
| N | % | Mean | SD | N | % | Mean | SD | N | % | Mean | SD | |
| N | 48 325 | 53 979 | 39 503 | |||||||||
| Women | 21 385 | 44.3 | 27 305 | 50.6 | 21 861 | 55.3 | ||||||
| Age | 48 325 | 45.7 | 15.9 | 53 979 | 48.6 | 15.6 | 39 503 | 54.5 | 15.2 | |||
| Education a | ||||||||||||
| Not graduated from secondary school | 38 809 | 80.3 | 34 957 | 64.8 | 20 247 | 51.3 | ||||||
| Secondary school graduate | 5485 | 11.4 | 11 551 | 21.4 | 11 261 | 28.5 | ||||||
| University degree (≥3 years) | 4031 | 8.3 | 7471 | 13.8 | 7995 | 20.2 | ||||||
| Occupation | ||||||||||||
| Higher grade professionals | 3664 | 8.0 | 3805 | 9.8 | 6347 | 16.3 | ||||||
| Lower grade professionals | 5777 | 12.6 | 7028 | 18.1 | 7735 | 19.9 | ||||||
| Routine nonmanual workers | 9566 | 20.9 | 8395 | 21.6 | 11 933 | 30.7 | ||||||
| Farmers | 7990 | 17.4 | 5123 | 13.2 | 2935 | 7.6 | ||||||
| Other self-employed | 3471 | 7.6 | 1882 | 4.9 | · b | |||||||
| Skilled manual workers | 6660 | 14.5 | 6305 | 16.2 | 7699 | 19.8 | ||||||
| Unskilled manual workers | 8692 | 19.0 | 6300 | 16.2 | 2247 | 5.8 | ||||||
| Currently working (part or full time) | 34 535 | 71.5 | 37 607 | 69.7 | 25 378 | 64.3 | ||||||
| Self-reported health good or very good | 38 006 | 78.8 | 40 184 | 75.0 | 28 337 | 73.9 | ||||||
| Long-lasting limiting illness c | 12 108 | 25.1 | 12 028 | 23.8 | 12 722 | 33.6 | ||||||
| Daily smoker | 17 384 | 36.3 | 15 033 | 29.2 | 6173 | 15.6 | ||||||
| HADS-A score | · | 52 867 | 4.2 | 3.3 | 39 383 | 4.0 | 3.3 | |||||
| HADS-D score | · | 53 516 | 3.4 | 3.0 | 39 465 | 3.3 | 2.9 | |||||
Prospective cohort study
The results of the prospective cohort study are shown in table 3. Male farmers had relatively low odds of psychological distress compared to most other occupational groups, whereas the odds for female farmers were similar to the odds for skilled manual workers and routine non-manual workers.
Table 3
The prospective association between occupation at baseline and symptoms of psychological distress, anxiety and depression 11 years later. The Nord-Trøndelag Health Study (HUNT). HUNT1 (1984–1986), HUNT2 (1995–1997) and HUNT3 (2006–2008). Baseline: HUNT1 (1984–1986) and HUNT2 (1995–1997). [OR=odds ratio; 95% CI=95% confidence interval.]
| Symptoms of psychological distress. Outcome measured in 1995–1997 a, b | Symptoms of anxiety caseness. Outcome measured in 2006–2008 c, d | Symptoms of depression caseness. Outcome measured in 2006–2008 c, e | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
||||||||||
| Men | Women | Both sexes | Both sexes | |||||||||
|
|
|
|
|
|||||||||
| N | OR | 95% CI | N | OR | 95% CI | N | OR | 95% CI | N | OR | 95% CI | |
| Higher grade professionals | 1251 | 1 | .. | 287 | 1 | .. | 2053 | 1 | .. | 2184 | 1 | .. |
| Lower grade professionals | 1155 | 1.20 | 0.88–1.63 | 2070 | 0.59 | 0.41–0.86 | 4018 | 1.13 | 0.89–1.43 | 4344 | 1.28 | 0.99–1.66 |
| Routine non-manual workers | 908 | 1.27 | 0.92–1.76 | 4054 | 0.72 | 0.51–1.02 | 4477 | 1.45 | 1.15–1.83 | 4902 | 1.78 | 1.38–2.28 |
| Farmers | 2135 | 1.09 | 0.82–1.44 | 1045 | 0.72 | 0.49–1.07 | 2735 | 1.47 | 1.15–1.88 | 2789 | 1.99 | 1.55–2.55 |
| Other self-employed | 999 | 1.19 | 0.86–1.64 | 354 | 0.80 | 0.50–1.28 | 864 | 1.41 | 1.02–1.94 | 925 | 1.83 | 1.32–2.54 |
| Skilled manual workers | 2391 | 1.14 | 0.87–1.50 | 292 | 0.67 | 0.40–1.11 | 2975 | 1.32 | 1.03–1.69 | 3110 | 1.84 | 1.44–2.36 |
| Unskilled manual workers | 1614 | 1.18 | 0.88–1.57 | 1683 | 0.90 | 0.62–1.29 | 2833 | 1.64 | 1.30–2.09 | 3073 | 1.84 | 1.42–2.38 |
Farmers had the second highest odds of having symptoms of anxiety caseness in 2006–2008. The odds ratios (OR) of symptoms of depression caseness were similar among the self-employed, routine non-manual workers, and manual occupational groups, at between 1.78 [95% confidence interval (CI) 1.38–2.28] and 1.84 (95% CI 1.42–2.38), and farmers had the highest odds, of 1.99 (95% CI 1.55–2.55).
Sibling study
The results of the sibling analyses are shown in table 4. Farmers and their siblings had virtually the same odds of having high levels of psychological distress in both 1984–1986 and 1995–1997. The odds of farmers having symptoms of anxiety were similar to those of their siblings in 1995–1997 [OR of siblings 0.98, 95% CI 0.84–1.15)]. In 2006–2008, the odds of anxiety caseness was 21% lower among siblings in other occupations than their farmer siblings (OR 0.79, 95% CI 0.63–1.00). In both surveys, farmers had higher odds of depression caseness than their siblings working in other occupations. Compared to farmers, siblings in other occupations had 25% decreased odds of depression in 1995–1997 (OR of siblings 0.75, 95% CI 0.63–0.89), and 30% decreased odds of depression in 2006–2008 (OR of siblings 0.70, 95% CI 0.55–0.89).
Table 4
Psychological distress, anxiety and depression caseness among farmers compared to their siblings working in other occupations. The Nord-Trøndelag Health Study - HUNT1 (1984 - 1986), HUNT2 (1995 - 1997) and HUNT3 (2006 - 2008). Adjusted for sex, age, education and birth order. [OR=odds ratio; 95% CI=95% confidence interval; Nobs=number of observations; Ngrp=number of groups (families); Naverage=average number of observations per group.]
| High level of psychological distress a | Symptoms of anxiety caseness b | Symptoms of depression caseness c | ||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
|
|
|
|
||||||||||
|
HUNT1 Nobs=1724 Ngrp==594 Naverage=2.9 |
HUNT2 Nobs=1723 Ngrp==608 Naverage=2.8 |
HUNT2 Nobs=2577 Ngrp==880 Naverage=2.9 |
HUNT3 Nobs=1419 Ngrp==524 Naverage=2.7 |
HUNT2 Nobs=2099 Ngrp==703 Naverage=3.0 |
HUNT3 Nobs=1145 Ngrp==425 Naverage=2.7 |
|||||||
|
|
|
|
|
|
|
|||||||
| OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | OR | 95% CI | |
| Farmers | 1 | · | 1 | · | 1 | · | 1 | · | 1 | · | 1 | · |
| Siblings | 0.95 | 0.78-1.15 | 0.99 | 0.82-1.21 | 0.98 | 0.84-1.15 | 0.79 | 0.63-1.00 | 0.75 | 0.63-0.89 | 0.70 | 0.55-0.89 |
Sensitivity analysis
The results of the sensitivity analyses are shown in the supplementary materials (www.sjweh.fi/index.php?page=data-repository). The results of analyses using the occupational group of the siblings are shown in supplementary table 2. The odds of farmers having high levels of psychological distress did not deviate substantially from other occupational groups and, with the exception of unskilled manual workers who had the highest odds in both 1984–1986 and 1995–1997, we did not find a clear socioeconomic gradient. For symptoms of anxiety caseness, farmers had similar odds to most other manual occupational groups in both 1995–1997 and 2006–2008, although they had the second highest odds in 2006–2008 (OR 2.24, 95% CI 1.19–4.24). Farmers had the highest odds of having symptoms of depression caseness in 1995–1997 (OR 1.62, 95% CI 1.00–2.63), and the second highest odds in 2006–2008 (OR 2.10, 95% CI 1.09–4.05). The results of analyses relating to full siblings only are shown in supplementary table 3 and support the main analyses. The results of analyses including siblings with a maximum age difference of 10 years are shown in supplementary table 4 and support the main analyses.
Discussion
In the prospective cohort study, we found that farmers had high odds of symptoms of depression compared to other occupational groups. In the sibling study, farmers had higher odds of having symptoms of depression compared to their siblings in 1995–1997 and 2006–2008 and higher odds of having symptoms of anxiety in 2006–2008. This might indicate that working in the agricultural industry may impact mental health.
Interpreting the findings in occupational studies is complicated due to several factors. Occupation is a commonly used way of measuring socioeconomic status (25), and occupation is thus a marker of socioeconomic factors that extend beyond the work environment alone. In addition, bias due to the “healthy worker effect,” which is caused both by selection of healthy individuals into work-life and unhealthy individuals out of work-life (26), makes interpretation of differences in health between occupations difficult. The healthy worker effect is likely to be more pronounced in physically demanding occupations (27), such as farming. Farmers are a particularly interesting and challenging occupational group to study, not only with regard to the health consequences of industry-specific challenges in agriculture and the possible selection processes related to the decreasing numbers of farmers, but also in terms of studying the consequences of high socioeconomic stress in the labor market in general. In addition, there is a unique way of acquiring the profession. Norwegian farms are family owned; by law, the firstborn child (before a change in the law in 1974, it was the firstborn son) is given priority to buy the family farm (28).
We found that farmers had higher odds of having symptoms of depression caseness compared to their siblings, and in 2006–2008 they also had higher odds of having anxiety caseness. Sibling comparison designs allow adjustment for unmeasured confounders shared by the siblings, and even though such studies cannot prove causality, they can support causal reasoning when also taking already existing knowledge and complementary analyses into account (11). To our knowledge, this study is the first to use a sibling comparison design to investigate the mental health of farmers. Two large cross-sectional studies found that Norwegian farmers had high levels of symptoms of depression (5, 6), and in our prospective analysis, we found that farmers had the highest odds of having symptoms of depression of all occupational groups in the study.
Confounding due to the healthy worker effect may be a possible explanation for the observed differences in the odds of having symptoms of depression in farmers and their siblings. To reduce this possible bias, we used the first known occupation in the sibling analyses. Although health-based selection into work-life still remains, we at least partially accounted for it by only including siblings with a known occupation in our analyses. An increased selection of siblings with symptoms of depression in farming appears unlikely even though it cannot be ruled out. There was a tendency for the firstborn to have lower odds of high levels of psychological distress, anxiety, and depression symptoms than younger siblings (results not shown).
Strengths and limitations
The HUNT study is one of the largest longitudinal population surveys in the world, and the participation rates were high, especially in the two first surveys. We had data on a large number of participants, many of whom had taken part in more than one survey. Further, our study population included participants who were no longer occupationally active, which may have reduced confounding due to the healthy worker effect (26).
The participation rate in the HUNT Study decreased in the period from 1984–1986 to 2006–2008 (13), which might have biased our results. The same trend is seen in other population-based epidemiologic studies worldwide (29). However, it is not the low participation rates themselves that introduce nonparticipation bias, but rather the extent to which nonparticipation is associated with the exposure or outcome of interest. Most studies have found that non-participation did not introduce substantial bias (29). In all three waves of HUNT, the most important self-reported reasons for non-participation in the study were lack of time or of interest (15,30,31). Ill health was the most important self-reported reason for non-participation only in the oldest age groups (>70–80 years) (15, 31). Non-participants in HUNT3 had lower socioeconomic status, higher mortality, and a higher prevalence of several chronic diseases than participants (31), indicating that some degree of selection bias is likely to have been present. Further, depression might be a more restricting factor for participation than anxiety (31), which might have led to an underestimation of our estimates of symptoms of depression, particularly in groups of low socioeconomic status. Any non-participation bias present would be expected to be most prominent in the prospective analyses, as the inclusion criteria demanded that a considerable amount of data needed to be available at two time points, as opposed to just one in the sibling study.
The sibling design is a further strength of our study. Non-shared confounding and random measurement error could still have biased the results (11). Non differential misclassification of a dichotomous exposure will bias the results towards the null (26), but the direction of possible bias caused by non-shared confounding is more difficult to predict. Under Norwegian law, sex and birth order play an important role when determining which sibling buys a family farm (28). There are most likely numerous other unmeasured factors involved in intergenerational transfer of farm properties, but it appears unlikely that having an early-life mental health problem will cause a sibling to be more likely to become a farmer.
We used national registry data to identify siblings. Parentage data might be missing for children or people who did not live in the same household as their parents at the time of the 1960 census, the records of which were the basis for the foundation of the National Registry in 1964 (32). The older participants in our study population are more likely to have had unidentified siblings than younger participants, and thus would not have been included in our siblings analyses. Further, we defined siblings as having the same mother, thus ignoring the genetic differences between half-siblings and full siblings. In addition, half-siblings with the same father were not included in our study. However, sensitivity analyses including full siblings suggest that any possible bias caused by our approach would have been minor.
Using screening tools as measures of psychological distress may be considered a weakness of our study. However, diagnostic interviews are not feasible in large-scale health surveys such as the HUNT study. Farmers also appear particularly reluctant to seek help for mental illness due to stigma (7), and this might have introduced bias if we had used diagnoses from medical records. Further, the mental health measurements in a total population-based study may be more reliable than an occupation-specific one, as participants may over-report mental health problems if they know they have been recruited to a study based on their occupation (33). Mental health was measured at two points that were 11 years apart. It is a limitation of our study that we do not know how many participants had developed a mental health problem after the first measurement, which was no longer prevalent at the time of the second measurement.
Another weakness of our study is that two different mental health measurement instruments were used in the three waves of the HUNT study. This makes studying the development of mental health over time difficult. Further, we found conflicting results using the two different measurement instruments. The ADI consists of only four questions and does not distinguish between anxiety and depression symptoms. This might have led to a possible difference in depression symptoms being obscured by the anxiety questions of the ADI. When validated against the HADS, the ADI had a lower sensitivity and a higher specificity than HADS, which has been validated and is used extensively in the literature, even though it has been criticized (34). We consider that the weaknesses of the ADI outnumber those of the HADS, and that it is likely that the results of the analyses using the HADS are more valid than the analyses using the ADI.
Occupational coding has changed over time, which is a limitation of our study. Misclassification may have biased our results in an unknown direction. Further, we only had data for the main occupation in HUNT1 and HUNT3. Farmers commonly have another off-farm job, and having data on such off-farm jobs would have strengthened the study. In HUNT2, data on all occupations were recorded, but – for participants stating that they had more than one occupation – we did not know which of them was primary. Our assumption that the occupation with the highest socioeconomic status would have had the main influence on their health might have been erroneous, especially if that occupation was not the participant’s main occupation. In addition, the EGP scheme uses characteristics of employment relations to classify occupations, and is thus not strictly hierarchal (25). In HUNT2, we used the EGP scheme in a hierarchal way for participants with several occupations, which might have been a weakness. However, only 8.6% of the HUNT2 participants had two or more occupations, and the majority had an occupational measurement in HUNT1. As a result, the impact on our estimates is probably low, as it only concerns a small proportion (3.1%) of the HUNT2 participants.
The population of Nord-Trøndelag County closely follows Norwegian trends in disability (35) and cause-specific mortality (36), and our results are likely to be generalizable to other rural parts of Norway with agriculture. The extent to which our results may be generalizable to agricultural populations in other industrialized countries is unknown due to differences in factors such as agricultural structure and healthcare or welfare policies, but they could be of interest internationally.
Concluding remarks
Farmers had higher odds of having high depression scores compared to both other occupational groups and their siblings who were not working as farmers. In the period 2006–2008, farmers also had higher odds of having high anxiety symptoms compared to their non-farmer siblings. This suggests that working in agriculture may impact mental health. Our findings may be of relevance in the agricultural industry as well as in clinical practice, occupational health services, and in agricultural and labor market policy-making. The results also indicate that there may be a need to develop and implement culturally appropriate initiatives to prevent, identify and treat mental health problems among farmers.



