Recently, the Danish Working Environment Research Fund commissioned us to undertake a systematic review of risk and prognosis of inguinal hernia in relation to occupational mechanical exposures. The Danish National Board of Industrial Injuries and the Occupational Diseases Committee requested the review for use in negotiations on the inclusion of new diseases in the list of occupational diseases and to adjust the practice regarding recognition of unlisted diseases caused by the particular nature of the work. This paper is a slightly revised version of the reference document that can be found on the website of the Danish National Board of Industrial Injuries (http://www.ask.dk/Arbejdsskadestyrelsen/~/media/D1CA5E01569744FEA53B9C8589CA8568.ashx). Existing Danish guidelines for recognizing hernias as unlisted diseases date back to 1997 (https://www.retsinformation.dk/Forms/R0710.aspx?id=84901).
An inguinal hernia is a protrusion of contents of the abdominal cavity through a defect in the lower abdominal wall above the inguinal ligament (1). Medial (or direct) hernias penetrate through a non-preformed gap, whereas lateral (or indirect) hernias pass through the inguinal canal. Lateral hernias may protrude within a patent processus vaginalis, which is an embryological evagination of the peritoneum. For both types of inguinal hernia, the main symptoms are pain and discomfort due to groin swelling. The most severe complication is incarceration of the hernia, which is a surgical emergency.
Inguinal hernia is far more common among men than women, with a reported age-adjusted male to female ratio of 7.5:1 (2). In terms of a swelling observed at clinical examination or a previous repair, inguinal hernia occurred with a lifetime prevalence of 15% among men aged ≥25 years (3). The lifetime prevalence increased with age from 5% in the age group 25–34 years, 10% in the age group 35–44 years, 18% in the age group 45–54 years, 24% in the age group 55–64 years, and 31% in the age group 65–74 years, to 45% among men aged ≥75 years (3).
Except in case of serious comorbidity, surgical treatment of symptomatic inguinal hernias is recommended, whereas watchful waiting may be an acceptable option for asymptomatic or minimally symptomatic hernias (1, 4). According to a register study from the United Kingdom, the all-ages annual incidence of inguinal hernia repairs was 13 per 10 000 in the period 1976–1986 (5), which probably underestimated the true incidence because surgery in private hospitals was not included (6). After the first year of life, the risk of inguinal hernia repair among males rose with age up to 65 years and declined slightly thereafter (5). Among male patients aged 15–39 years, 78% of operated inguinal hernias [excluding combined medial and lateral hernias (pantaloon hernias) and hernias with unknown type] were lateral (7). This percentage was 60% for the age group 40–59 years and 55% for men aged ≥60 years (7). Around one fourth of all men can expect to have an inguinal hernia repair at some point (2, 5), and men account for 90–95% of all inguinal hernia repairs (5, 8, 9).
Potential risk factors include a family history of inguinal hernia (10–12), comorbidity such as prostatic hypertrophy (3) and chronic obstructive pulmonary disease (11), ethnicity (2), and smoking (1), whereas a high body mass index seems to have a protective effect (2, 3, 12, 13). Heavy physical workload (14, 15) and standing for long periods at work have been implicated as risk factors (http://www.mayoclinic.com/health/inguinal-hernia/DS00364/DSECTION=risk%2Dfactors). Potentially, a single strenuous event may also induce an inguinal hernia. Although there may be little clinical merit in differentiating between medial and lateral hernias (1, 16), the influence of occupational risk factors may differ.
Several surgical techniques are used that can be broadly categorized as open (sutured or mesh) or laparoscopic (17). Historically, open techniques were the first to be applied, whilst laparoscopic techniques did not gain a foothold until after around 1990. Open techniques are most commonly used. Hernia recurrence and persistent pain are considered the most important adverse outcomes following inguinal hernia repair. The question is if generically or quantitatively different occupational mechanical exposures are related to different probabilities of these outcomes. In Denmark, around the millennium, 17% of all inguinal hernia repairs were performed due to recurrence (18). The risk of recurrence depends on surgical technique (lower risk after mesh than non-mesh techniques) (19, 20) and maybe also on defective collagen metabolism (21). Persistent pain for months or even years is a common symptom after inguinal hernia repair (22–26). In a Danish patient population, pain impairing daily activities was reported in 17% one year after open inguinal hernia repair (27) and in 6% after 6.5 years (28). In addition to surgical technique (eg, laparoscopic techniques seem to convey a lower risk than open techniques) (24, 25, 29), surgery for recurrence (24, 25), young age, female gender, preoperative chronic pain, and acute pain in the early post-operative period have been identified as risk factors (22, 30). Psychological factors may also play a role (30, 31).
Another important prognostic outcome is duration of post-operative sickness absence that has considerable economic implications for society. In part, however, this outcome reflects advice on convalescence (32) that has traditionally depended on surgery type (open or laparoscopic) and expected physical strain at work (33, 34). Therefore, standardized recommendations on (early) return to work are a prerequisite for valid comparisons of patient groups with respect to the length of time necessary before the patient can resume work following inguinal hernia repair (35). Even when surgeons provide standardized recommendations on early return to work, this may not be followed by the patients (eg, due to contrary advice from general practitioners or employers). A priori, it therefore seems difficult to extract meaningful information on prognosis in relation to occupational mechanical exposures from studies that focus on duration of post-operative sickness absence as an outcome in its own right. In studies on risk of recurrence and persistent pain, prolonged post-operative sickness absence may be a protective factor, which should be taken into consideration. These arguments are reflected in the way we delineated the present review of the literature on prognosis.
Our overall objective was to produce a systematic review in the form of a reference document evaluating the epidemiologic evidence for (i) causal relations between occupational mechanical exposures and the development of lateral and medial inguinal hernia and (ii) effects of occupational mechanical exposures on post-operative prognosis. Specific objectives were to present exposure–response patterns for associations that were likely to be causal and evaluate the risk of hernia recurrence and persistent post-operative pain in relation to early return to work characterized by different mechanical exposures. Part of the objective was to assess any impact of gender on these relationships. In case of insufficient evidence, a further objective was to outline major research needs.
Methods
Literature search
We conducted a systematic search in Medline (last updated 3 November 2011) using the terms (inguinal hernia OR hernia repair OR (inguinal hernia AND recurrence) OR (inguinal hernia AND reoperation) OR (inguinal hernia AND pain)) AND (convalescence OR work OR occupation OR strenuous OR occupational exposure OR lifting OR physical load OR standing OR walking OR work related OR occupational epidemiology OR risk factor*). Corresponding searches were performed in Embase and Web of Science. Moreover, we searched the reference lists of retrieved original papers and reviews for additional relevant material. Duplicates were excluded.
Selection of articles
First based on the title and second based on reading of the abstract, two researchers selected candidate papers to be retrieved in fulltext. Any differences of opinion were resolved through consensus. Included papers had to (i) be in English, Scandinavian, French, or German, (ii) be published in a peer-reviewed journal, (iii) describe results of an original study, and (iv) comprise an analysis of risk or prognosis of inguinal hernia in relation to occupation or occupational mechanical exposures. We excluded risk studies that did not include a control group. However, we made an exception from this criterion with respect to the potential impact of a single strenuous event where we included case series because we identified no other types of study. Case series that only considered compensation cases were excluded, and we did not include case reports. Prognostic studies with duration of sickness absence as the only outcome were excluded.
Article review
For each article on risk of inguinal hernia that we finally reviewed, we tabulated a standardized set of information on study design, population and completeness of participation, outcome assessment, exposure assessment and exposure contrasts, effect estimates [with 95% confidence intervals (95% CI) or P-values], and confounder adjustment. For each article of prognosis with respect to recurrence, we tabulated study design, population and completeness of participation, type of hernia, surgical technique, assessment of recurrence, exposure assessment, effect estimates (with 95% CI), and outcome probabilities given the exposure in combination with other predictors. Where counts or prevalence estimates were provided without any effect estimates, we calculated risk differences or odds ratios (OR) with exact 95% CI using STATA 11.2 (StataCorp, College Station, TX, USA).
A brief description of each original study is below, together with an evaluation of each study’s contribution to knowledge. The evaluations were based on a qualitative rating that considered limitations of design, potential for bias (inflationary or towards the null), adjustment for potential confounders (in studies of risk), inclusion of relevant potential predictors in multivariable models (in studies of prognosis), appropriateness of statistical analyses, and power to detect associations under study.
Grading of evidence for causal and prognostic relations
Across the individual articles on risk of inguinal hernias (or hernia repairs), we rated the degree of evidence for a causal association between a given exposure and a defined outcome according to the framework of the Scientific Committee of the Danish Society of Occupational and Environmental Medicine that has been adopted by the Danish Working Environment Research Fund (see the appendix). We based the grading on the quality, consistency, and amount of evidence. The evidence for prognostic relations between occupational mechanical exposures and post-operative outcomes was evaluated according to the same framework, replacing the word “causal” with “prognostic”. We were interested in causal associations between risk factors and negative prognostic outcomes, rather than prediction per se (36, 37). Therefore, we considered confounding relevant in prognostic studies.
A note on terminology
In the surgical literature on inguinal hernias, the term “primary” is used to designate a hernia that occurs for the first time or a first-time hernia repair. However, in other areas of surgical literature, “primary” has other connotations: eg, primary osteoarthritis means osteoarthritis of unknown aetiology as opposed to secondary osteoarthritis that occurs due to other disorders or trauma. We chose the term “first-time” to designate first-time occurrences.
Results
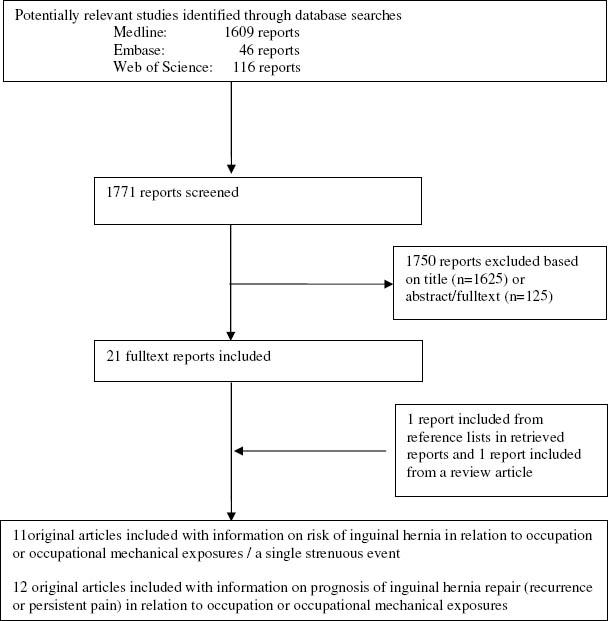
Figure 1 illustrates the literature search. The search revealed 1771 reports, of which 1625 were excluded based on title and 125 were excluded based on abstract or fulltext. A total of 23 original papers were included, including 1 (38) that was identified through the reference list in another paper (39), and 1 (40) that was identified in a review (34). Of the 11 original papers on risk, 8 assessed the risk of inguinal hernia in relation to occupation or occupational exposures (2, 3, 11, 12, 38, 39, 41, 42) and 3 assessed the risk of inguinal hernia in relation to a single strenuous event (43–45). Of 12 original papers on post-operative prognosis, 7 concerned recurrence (35, 40, 46–50) and 6 concerned persistent pain (49, 51–55); 1 provided results on both outcomes (49).
Figure 1
Flowchart on stages of identification, screening, and selection of studies investigating risk and prognosis of inguinal hernia in relation to occupation or occupational mechanical exposures.
Risk of inguinal hernia by occupation or occupational mechanical exposures
Of the eight epidemiologic studies with information on risk of inguinal hernia in relation to occupation or occupational mechanical exposures, three were cross-sectional (3, 38, 39), four were case–control studies (11, 12, 41, 42), and one was a prospective cohort study (2). Four studies included only men (3, 11, 38, 39), two studies included around 80% men (41, 42), one study included 40% men (2), and one study included only women (12). Two studies relied on self-reported outcomes (38, 39), two studies were based on physician diagnoses (2, 3) in part reported by the participants (2), and the four case–control studies focused on hernia repair (11, 12, 41, 42). Among the six studies that did not rely on self-reported outcomes, four studies focused on inguinal hernias (2, 3, 11, 12), and two studies included femoral hernias together with inguinal hernias (41, 42). Only two studies were explicitly restricted to first-time inguinal hernias (2, 11). Exposure assessment was based on self-reported work activity levels in four studies (2, 3, 11, 12), a combined measure for self-reported work and leisure-time activity levels in one study (41), job titles in two studies (38, 39), and a job exposure matrix (JEM) with three (3) or four (42) exposure categories in two studies. Two studies adjusted for potential confounders (2, 3), but only one study presented adjusted risk estimates (2). The main characteristics and results of the eight studies are presented in table 1. The brief descriptions that follow are arranged first by year of publication, second alphabetically according to the first author’s surname.
Table 1
Main characteristics and results of eight epidemiologic studies on risk of inguinal hernia by occupation or occupational mechanical exposures. The studies are ordered first by publication year and second alphabetically according to the first author’s surname. [OR=odds ratio; 95% CI=95% confidence interval; RR=risk ratio; SD=standard deviation]
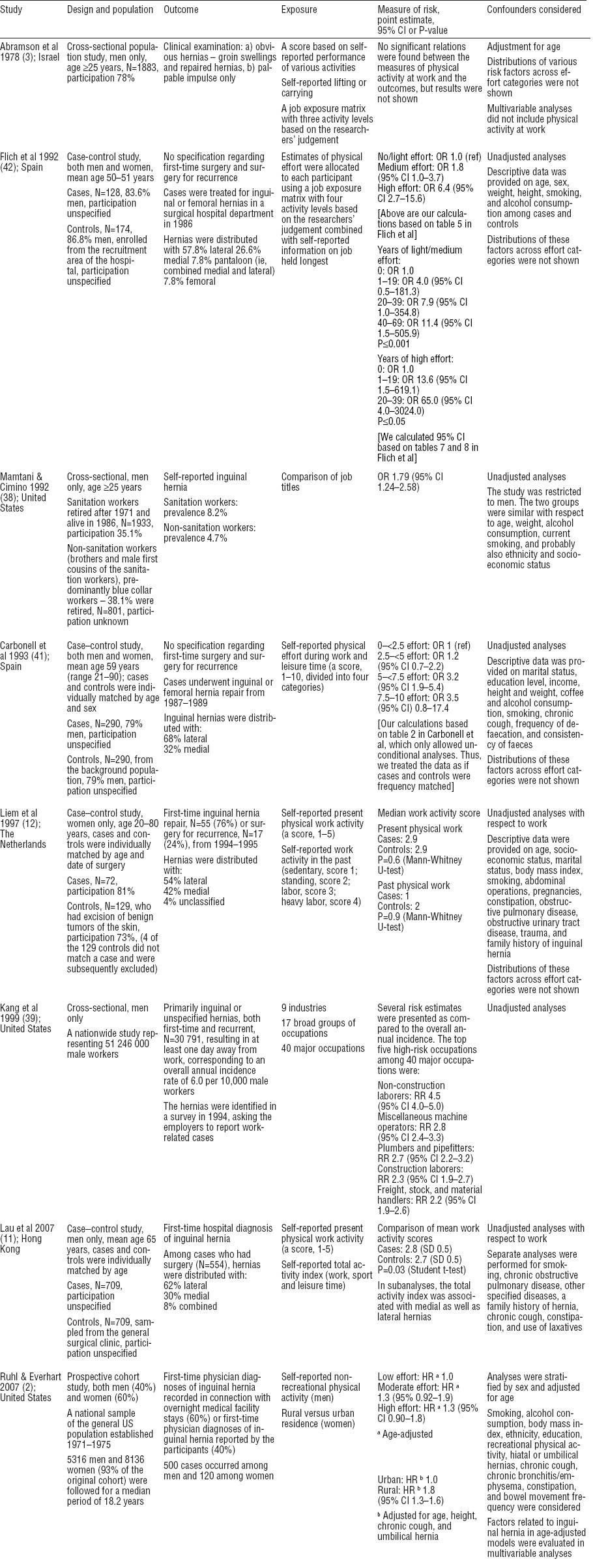

Abramson et al (3) conducted a cross-sectional population study that entailed clinical examination of 1883 men aged ≥25 years. Physical activity at work was assessed by (i) a score based on self-reported performance of various activities, (ii) self-reported frequency of lifting and carrying, and (iii) a 3-level JEM, where the researchers classified all jobs as light (eg, bus driver, clerk), active (eg, postman, carpenter), or heavy (eg, boilermaker, dock laborer) (56). No significant associations were found between inguinal hernia and physical activity at work, but this statement was not substantiated by any risk estimates. A particular strength of this study was that it was based on clinical examination of a population sample rather than relying on self-reported outcomes or being restricted to cases diagnosed at a hospital. A further strength was independent exposure assessment in addition to self-reported estimates. Unfortunately, physical activity at work was not included in multivariable models, and risk estimates were not presented.
Flich et al (42) compared 128 cases who were surgically treated for inguinal or femoral hernia with 174 controls from the recruitment area of the hospital. Exclusion criteria for cases and controls differed in that controls were excluded if they had a clinical history of any kind of hernia or “closely-related illnesses”. Exposure assessment was based on self-reported information on the job held longest combined with a JEM comprising the researchers’ ratings of intensity of physical effort. Possible ratings were (i) no effort or sedentary work (eg, night watchman, office worker), (ii) light effort: standing work involving occasional lifting of not-too-heavy weights (eg, waiter, shop assistant, electrician), (iii) medium effort: more frequent lifting (eg, agricultural and construction workers, cleaners), and (iv) high effort: daily effort (eg, quarry workers, manual warehouse workers). Duration of employment with these four effort intensities was also investigated. Findings suggested exposure–response relations both for exposure intensity and duration and the risk associated with duration of exposure was larger for years of high effort than years of light/medium effort (table 1). The results were not adjusted for any confounders. The main strength of this paper was the independent exposure assessment that minimized any risk of recall bias. However, the exposure characterization was limited, and no confounder control was made; the fact that cases and controls did not differ significantly with respect to mean age does not preclude this source of distortion of the risk estimates. Still, the increased risk associated with duration of exposure to high efforts when compared to light/medium efforts cannot be explained by age as a confounder.
Mamtani & Cimino (38) compared retired sanitation workers with non-sanitation workers of whom 38.1% were retired. The study was cross-sectional. Around one third of the sanitation workers participated, whilst the proportion who participated among non-sanitation workers was unknown. The two groups were compared with respect to 17 illnesses that were assessed by self-report (results for stomach/gastric ulcer seem to be duplicated). Among sanitation workers, the prevalence of inguinal hernia was 8.2% versus 4.7% among non-sanitation workers. It is not clear whether these percentages represented point or lifetime prevalence. It seems likely that sanitation workers were more exposed to heavy lifting than non-sanitary workers, but probably some of the non-sanitation workers were also exposed to heavy lifting (11.4% were employed in craft and repair). This study had several limitations: low participation, cross-sectional design, self-reported outcome, weak exposure characterization, and multiple comparisons. Non-sanitation workers were exposed to some extent, which may have led to lower risk estimates than if the comparison group had been “unexposed”. On the other hand, the restriction to former sanitation workers probably implied selection of unhealthy workers into this study group and low participation in this group may have further exaggerated this source of bias to the extent that symptomatic sanitation workers were more likely to participate. Thus, it seems likely that inflationary bias explained the increased risk for sanitation workers.
Carbonell et al (41) performed a case–control study of 290 cases who underwent inguinal or femoral hernia repair, and 290 individually age- and sex-matched controls from the recruitment area of the hospital. Exclusion criteria for cases and controls differed in that controls were excluded if they had previously had surgery for any kind of hernia, not just the hernia types under study. Among males, 9.6% (22/228) of the cases had a femoral hernia repair. Among females, this percentage was 69% (43/62). Exposure assessment was based on an interview with subsequent calculation of an effort score (1–10) that reflected physical activity during work and leisure time. The calculation of the score was inadequately described, and there seems to be logical inconsistencies in its construction: physical exertion only at work, only during leisure time, and both at work and during leisure time were all scored 1=yes and 0=no, implying that all participants would be allocated a total of 1 score point for these 3 items. The mean effort score (presumably in the most recent job) was significantly higher among cases than controls (5.06 versus 3.21, table 1 in Carbonell et al). The effort score for the most recent job was then divided into four categories, but only one unadjusted OR of 2.92 was reported (95% CI 2.11–4.04, table 5 in Carbonell et al). According to our calculations, OR increased with increasing category of effort (table 1). Despite the matching, the authors reported an OR for sex of 0.98 (table 5 in Carbonell et al). This study had many limitations. The statistical analyses were not transparent and did not inspire confidence. Different outcomes were lumped together. Occupational exposures were poorly characterized and – most importantly – the effect measures may well be overestimated due to recall bias (cases may have been more likely to overestimate their exposures than controls).
Liem et al (12) conducted a case–control study among women who underwent inguinal hernia repair (cases) or surgery for benign skin tumors (controls). The analyses included 72 cases and 125 controls who were individually matched to the cases by age and time of surgery. Exposure assessment was based on questionnaire data, and present and past work activity intensities were scored 1–5 and 1–4, respectively. Furthermore, cumulative measures were calculated by multiplying activity score and duration of employment (years); this was done separately for present and past activity. Selection of variables for inclusion in the final multivariable conditional regression analysis was guided by univariable unmatched significance testing of uneven distributions between cases and controls. In this way, occupational exposure variables were excluded from the final model. Based on small numbers, it was noted that climbing stairs was protective. A strength of the study was the sampling frame that probably ensured that the controls were included independently of occupational exposures and that controls would have occurred as cases had they developed an inguinal hernia. In addition to a relatively large proportion of recurrent hernias, major limitations were the small study size and the method used to select variables for the final model, which meant that the study may well have overlooked associations. The seemingly protective effect of climbing stairs may be an example of reverse causation.
Kang et al (39) reported results from a cross-sectional study of hernias (N=30 791, primarily inguinal or unspecified) that employers identified as work-related. The study was restricted to men. One-year cumulative incidences were calculated by industry and occupation categories, and relative risks were presented using the incidence for the total population of 51 246 000 male workers in private industries, mines, and railways as a reference. The estimates were not adjusted for age or other factors. The highest relative risks were found in occupations with strenuous, heavy manual labor. By focusing on inguinal hernias that were judged to be work-related, this study reflected widespread beliefs regarding risk factors for inguinal hernias (which the authors remarked) as well as compensation practices. Thus, the results do not represent valid estimates of the risk of inguinal hernias according to industry and occupation.
Lau et al (11) conducted a case–control study among men. A total of 709 cases with a first-time hospital diagnosis of inguinal hernia were compared with 709 individually age-matched controls, sampled from the hospital’s general surgical clinic. Present work activity intensities were scored 1–5 by means of a questionnaire. Between cases and controls, a statistically significant difference in mean work activity score of 0.1 was observed. No OR were presented for the work activity index, which does not seem to have been considered for multivariable analysis. There were several limitations in this study. The appropriateness of the control group could not be judged [eg, varicose veins may share risk factors with inguinal hernia (3) meaning that inclusion of patients with varicose veins in the control group would lead to underestimation of effects], and in particular, there was a potential for inflation of observed associations due to recall bias. Even if correct, it must be questioned if the small difference between cases and controls with respect to the work activity score was clinically important.
Ruhl & Everhart (2) reported results from a prospective cohort study (NHANES I) that comprised 13 452 persons, who were followed for a median period of 18.2 years with respect to first-time inguinal hernia diagnoses made by a physician. For men, the analyses included baseline interview data on non-recreational activity, classified as inactive (11.4%), moderately active (44.5%), and very active (44.1%). Criteria for this classification were not stated. For women, the analyses included rural versus urban residence. It is unclear why urbanicity was not included in the analyses for men, and why activity level was not included in the analyses for women. In Cox proportional hazards analyses, age-adjusted hazard ratios for activity level were insignificant for men, and this variable was not included in the final model. For women, rural residence was significantly related to the outcome. This study benefitted from a longitudinal design, a large sample, a high participation at follow-up, physician-based diagnoses, and consideration of several potential confounders. However, 44% of the population was classified as having a very active non-recreational activity level, which suggests that the exposure contrast between categories was limited. It may also be questionable if the activity level at baseline represented the activity level throughout the whole period. Rural residence is a dubious proxy for high physical activity. Hence, for the purpose of the present review, the exposure assessment was weak and exposure misclassification could easily have biased estimates of associations towards the null.
Risk of inguinal hernia in relation to a single strenuous event
The risk of inguinal hernia in relation to a single strenuous event was addressed in three case series that included a total of 582 surgical patients (43–45). Two studies were not restricted to first-time inguinal hernia, but included recurrent hernias (43, 45) and other types of hernia (43). The proportion of patients who reported a sudden onset ranged from 7% and 11% to 43%, and patients with a sudden onset tended to relate their hernia to a specific strenuous event.
Smith et al (45) reported results from a series of 129 patients (95% men) who were seen at a surgical department due to first-time (74%) or recurrent inguinal hernia (26%) over a six-month period (calendar year not specified). It is unclear whether an interview or questionnaire was used to collect the data. Participation was not stated. None of the patients were engaged in claims for industrial injury compensation, but it is unclear whether this was an exclusion criterion. Seven percent (N=9) of the patients reported a sudden onset related to: lifting strains at home or at work (N=8), or a fall (N=1). The sudden onset hernias were all first-time occurrences and they were medial in five cases, lateral in three cases, and of unknown type in one case. For the gradual onset group, the numbers with lateral and medial hernias were not reported. The study reflected beliefs regarding risk factors for hernias, rather than evaluating if anything unusual took place shortly before the onset.
Pathak & Poston (43) reported questionnaire-based results from a series of 133 patients with 135 inguinal (85%) or other abdominal hernias (15%), 19% of which were recurrent. The patients were seen at a general surgical hospital clinic over a 6-month period in 2003. Participation was 99%; the distribution between males and females was not reported. Eleven percent (N=14) of the patients reported a sudden onset caused by: a single strenuous or traumatic event in terms of heavy lifting at work (N=1), strenuous exercise and stretching (N=3), coughing (N=2), or an unidentified activity (N=8). No distinction was made between medial and lateral hernias. The study reflected beliefs regarding risk factors for hernias, rather than evaluating if anything unusual took place shortly before the onset.
Sanjay & Woodward (44) reported questionnaire-based results from a series of 320 patients who underwent inguinal hernia repair from 1995–2004. Only first-time hernias were included. Participation was 62% (320/520); the distribution between males and females was not reported. Forty-three percent (N=137) reported a sudden onset. Lateral hernias were diagnosed among 74% of the patients with a sudden onset and among 57% of patients with a gradual onset (P<0.05). In the group with a sudden onset, 31% (42/137) reported heavy work; the corresponding percentage in the group with a gradual onset was 9% (14/163) (for heavy and manual work combined, the percentages were 46% and 17%, respectively, P<0.05). Patients with a sudden onset thought that a single strenuous or traumatic event caused their hernia in terms of one of four pre-specified response options: lifting (N=93), coughing (N=20), exercise (N=14), and gardening (N=10). The study reflected beliefs regarding risk factors for inguinal hernias, rather than relations to unusual events that took place shortly before the onset. The long recall period of up to nine years and the prespecified response options probably increased the risk that patients rationalized after the fact. The hernia may also have been present, but unnoticed by the patient before an event that provoked symptoms (57). However, these sources of error could not explain the finding that lateral hernias were more likely to have a sudden onset than medial hernias, nor the increased occurrence of a sudden onset among patients with heavy work. If corroborated, these observations might suggest an injury mechanism where increased intraabdominal pressure makes the hernia protrude preferentially through the preformed canal.
Post-operative prognosis by occupation or occupational mechanical exposures
Twelve studies were on prognosis: one concerned patients treated laparoscopically (40), and three concerned patients who were treated either laparoscopically or by open surgery (49–51) – two of which presented results from the same trial (50, 51). The remainder of the studies concerned patients who had open surgery (as judged from publication year, if not stated explicitly). Duration of post-operative sickness absence was considered in seven studies (35, 46–48, 50, 51, 53), but was not described in relation to occupational exposures in two of these studies (50, 51). In three studies, part of the patients received standardized advice on short post-operative sickness absence (35, 46, 48). Five studies did not take account of duration of post-operative sickness absence (40, 49, 52, 54, 55). The brief descriptions that follow are arranged first according to prognostic outcome (recurrence or persistent pain), second by year of publication, and third alphabetically according to the first author’s surname. The seven studies on recurrence (35, 40, 46–50) are also presented in table 2.
Table 2
Main characteristics and results of seven epidemiologic studies on prognosis with respect to recurrence after inguinal hernia repair by occupation or occupational mechanical exposures. The studies are ordered first by publication year and second alphabetically according to the first author’s surname. [95% CI=95% confidence interval; OR=odds ratio]

Post-operative prognosis with respect to recurrence
Ross (47) conducted a four-year follow-up study of hernia recurrence among 260 adult male patients who underwent surgery for first-time or recurrent inguinal hernia. As judged from the publication year (1975), the study concerned open repair. A total of 22 hernias (8.5%) recurred. Results were presented by means of a figure showing the distribution of patients and recurrences according to number of weeks off work and occupational exposures classified as light work (eg, office work), medium work (eg, shop keepers, sales representatives), or heavy work (eg, laborers, welders, butchers). No statistical analyses were performed. Based on our readings from the figure, the median time until return to work was 5, 6, and 8 full weeks in the 3 exposure categories, respectively, and 75.7% (84/111), 52.6% (50/95), and 20.4% (11/54) of the patients in the 3 exposure categories had returned to work after 6 full weeks. Among patients with light work who returned to work before 6 full weeks, 4.8% had a recurrence, and among patients with light work who returned to work after 6 full weeks, 3.7% (1/27) had a recurrence. Among patients with medium or heavy work who returned to work before 6 full weeks, 11.5% (7/61) had a recurrence, and among patients with medium or heavy work who returned to work after 6 full weeks, 11.4% (10/88) had a recurrence. As the author stated, early return to work (which we have interpreted as return to work before 6 full weeks after surgery) did not seem to increase the risk of hernia recurrence, and this applied whether the patients returned to light, medium, or heavy work. However, our readings and calculations showed that medium and heavy work was associated with a risk of recurrence of 11.4% (17/149) against 4.5% (5/111) for light work, yielding a univariable risk difference of 6.9% (95% CI 0.51%–13.3%; our calculation was based on the assumption that all patients had the same follow-up time – if recurrences occurred earlier in the exposed group, this assumption would lead to a conservative estimate of the risk ratio). The study was observational, and patients may have adjusted their convalescence so that symptoms and workload were balanced in a way that minimized the risk of recurrence. Results may not be generalizable to situations where all patients are expected to return to work early. Medium and heavy work was associated with an increased risk of recurrence irrespective of time off work, which suggests that prolonged convalescence did not sufficiently protect against the increased risk.
Bourke et al (46) reported results of a randomized controlled trial comparing an intervention group that was advised to return to full activity as early as possible and a control group who received usual advice on convalescence. Male patients were enrolled in the study 2–3 weeks after an inguinal hernia repair that was performed from 1976–1981. Judging from the surgery years, the study concerned open repair. After one year, 491 patients (95%) were followed up. In the intervention group 3.3% (8/246) had a recurrence as compared to 4.1% (10/245) in the control group; this difference was not significant. The intervention shortened the median convalescence from 65 to 48 days in comparisons restricted to workers (N=369). In the intervention group, patients with light (no lifting), intermediate (light lifting), and heavy work (heavy lifting) returned to work after a median of 42, 50, and 51 days, respectively. Among patients with heavy work, 3.5% (3/85) had a recurrence in the intervention group versus 1.1% (1/95) in the control group, and the corresponding univariable risk difference was 2.5% (95% CI -2.0%–6.9%; our calculation). Overall, shorter convalescence was not significantly related to an increased risk of recurrence. Due to small numbers, it was not possible to evaluate if earlier return to work was associated with a higher probability of recurrence among patients with heavy work.
Taylor & Dewar (48) conducted two randomized controlled trials from 1978–1980 focusing on hernia recurrence in relation to duration of post-operative sickness absence and type of work. One trial comprised 96 presumably male naval and marine officers (participation 100%) who were ordered to resume full duties either 3 weeks or 3 months after an uncomplicated open inguinal hernia repair (the study received ethical approval, but it seems that the officers were not asked for consent to participate). The other trial comprised 119 male civilians (participation 91%) with unspecified jobs who underwent the same type of surgery and who were either advised to resume work after 3 weeks or received usual advice. In both trials, the patients’ type of work was classified as heavy, light, or sedentary. Among the officers, 34% had heavy work, 49% had light work, and 17% had sedentary work. Among the civilians these percentages were 28%, 25%, and 47%. Recurrence within one year did not differ, but only two recurrences were observed. The trials were underpowered to detect differences between the intervention and control groups with respect to recurrence.
Le et al (40) conducted a follow-up study of 196 patients who were clinically examined on average 34 months after laparoscopic repair of a first-time (89%) or recurrent (10%) inguinal hernia or a femoral hernia (1%). Surgery was performed from 1996–1997. At follow-up, information was collected on “sustained physical activity”; it is not clear whether this information could be retrieved from clinical files or was obtained by a retrospective interview. No distinction was made between physical activity at work or during leisure time, and the timing of the physical activity in relation to surgery was not specified. Duration of post-operative sickness absence was not described. Among patients with sustained physical activity, 30.3% (10/33) had a recurrence, whereas among patients without such activity, the percentage was 14.7% (24/163). Thus, the univariable risk difference was 15.6% (95% CI -1.0%–32.2%; our calculation assuming that all patients had the same follow-up time, see above). Among patients with a recurrent hernia, 68% (23/34) were asymptomatic; this percentage was not specified according to physical activity. Multivariable analyses were not performed. Results suggested that sustained physical activity is a risk factor for recurrence after laparoscopic hernia repair. However, recall bias may have inflated the risk difference, and the result is difficult to interpret because of the unspecified timing and character of the physical activity.
Bay-Nielsen et al (35) advised 1084 men who underwent elective, open repair (with mesh) of a first-time inguinal hernia to return to work and daily activities on the day after surgery. The intervention period was 1999–2000. Among the 1059 men (98%) who provided preoperative questionnaire data, 646 were employed or self-employed. They classified their occupational physical activities as: “sedentary work” (22%), “walking, no heavy lifting” (28%), “intermittently strenuous work” (33%), or “constantly strenuous work” (14%). For the remainder, occupational physical activities were unspecified (5%). The median time off work ranged from 4.5–14 days for patients in the lowest and highest occupational exposure categories, respectively. One month after surgery, 25% of the patients with constantly strenuous work were still sick-listed as compared with 10% of the patients with sedentary or walking work with no heavy lifting. Pain and wound problems were the most common reasons for delayed resumption of work. All 1059 participants were compared with 1306 eligible patients who had surgery in the participating departments, but were not included in the study for administrative reasons, and with 8297 patients who had surgery in other departments. The two comparison groups were not characterized with respect to age, physical strain at work, or time off work after surgery. Within a median follow-up time of 16–17 months, reoperation rates did not differ between the 3 groups of patients. Reoperation rates were calculated as Kaplan-Meier estimates and compared with the log-rank test. The study indicated that patients with physically strenuous work had a longer period of convalescence after inguinal hernia repair than patients whose work was not strenuous, even though standardized advice on early return to work was given. While in general reassuring with respect to hernia recurrence in relation to early return to work among patients treated by an open repair technique, the most highly exposed group was small, the comparisons across groups were not stratified by exposure category, and the longer periods off work among patients with physically strenuous work may have had a protective effect. Hence, the study may have overlooked an increased reoperation rate among patients with constantly strenuous work.
Arvidsson et al (50) reported results of a randomized trial comparing two surgical techniques (laparoscopic repair versus open repair without mesh). From 1993–1996, 1068 male patients aged 30–70 years were enrolled in the trial in connection with first-time surgery for unilateral inguinal hernia. A total of 920 (86%) patients were followed up by an independent observer after five years or had developed a recurrence during follow-up. At baseline, patients were categorized as occupied in a job with light (39%), moderate (20%), or heavy physical exposures (23%), or as unoccupied (4%), retired (12%), or having an unspecified occupational status (1%). Median sick leave was 11 and 12 days in the two surgery groups, respectively. Duration of sick leave was not described in relation to occupational physical exposures. In a nonlinear mixed model analysis, occupational exposure status was not a prognostic variable for recurrence after either type of surgery (it is unclear if the analysis was uni- or multivariable). The result was reassuring, but exposure assessment was crude, which may have masked negative effects of specific exposures. To the extent that patients with heavy exposures had longer sick leave, a protective effect of sick leave would also tend to obscure any negative impact of occupational exposures on prognosis.
Post-operative prognosis with respect to recurrence and persistent pain
Matthews et al (49) followed 1696 men [participation 86% (1696/1983)] for two years after open (N=834) or laparoscopic (N=862) repair of a first-time or recurrent inguinal hernia performed from 1999–2001 (58). Information on physical activity level was collected by a preoperative questionnaire. A higher preoperative activity level (“active” versus “sedentary”) during work or leisure time predicted a higher risk of reoperation after a laparoscopic repair (adjusted OR 1.89, 95% CI 1.41–2.51; we calculated this result taking exp(x) of the values for beta and confidence limits, table 6 in Matthews et al). Physical activity level did not predict reoperation after open repair. Patients who reported that their highest physical activity level during work or leisure-time was moderate, heavy, or very heavy had a lower risk of pain exceeding three months after a laparoscopic repair than patients who reported their activity level to be light (adjusted OR 0.52, 95% CI 0.30–0.89). Physical activity level did not predict long-term pain after open repair. Duration of post-operative sickness absence was not taken into account. This study benefitted from prospective data collection and from separation of the two surgical procedures and the two post-operative outcomes. Results suggested that a higher than light activity level could be associated with a higher risk of reoperation, but a lower risk of persistent pain after a laparoscopic repair. Physical activity level did not predict reoperation or long-term pain after open repair. However, the crude assessment of physical activity levels was a weak point.
Post-operative prognosis with respect to persistent pain
Salcedo-Wasicek & Thirlby (53) conducted a follow-up study of 44 male patients with a mean age of 46 years who underwent first-time inguinal hernia repair in 1992, using an open technique (the study was not a matched case–control study, although the authors stated so). The outcomes were number of days to pain-free status and number of days until return to work according to a telephone interview. Standardized advice on early return to work was not given. The number of days off work was higher among patients with workers’ compensation than those with a commercial insurance. Both type of insurance coverage (workers’ compensation versus a commercial insurance) and self-reported work level (sedentary, moderate, or heavy lifting) were included in a multivariable Cox proportional hazards regression analysis. Type of insurance coverage was reported as the only significant prognostic factor with respect to duration of pain (hazard ratios were not reported). However, type of insurance coverage and work level correlated. Among patients with a workers’ compensation, 4% had sedentary work, 32% had a moderate work level, and 64% performed heavy lifting. Among patients with a commercial insurance, the corresponding percentages were 64%, 18% and 18%. Incidentally, the percentage with lateral hernias was 73% among patients with a workers’ compensation versus 55% among patients with a commercial insurance. It is a challenge to interpret results of multivariable analyses that include highly correlated variables, and the study could not disentangle effects of workers’ compensation and heavy work. The results may suggest that preoperative heavy work was associated with post-operative pain. Alternatively, the results may suggest that attempts to return to heavy work aggravated or perpetuated post-operative pain, or that the patients omitted early return to work because they expected aggravated symptoms or hernia recurrence. Therefore, the study is hardly informative for the purpose of the present review.
Poobalan et al (55) conducted a follow-up study among 226 patients (participation 64%, mean age 61 years, unspecified gender distribution) who had undergone open surgery (with or without mesh) for first-time or recurrent inguinal hernias from 1995–1997, ie, 21–57 months previously. They were asked to recall pain lasting >3 months after the operation and to state their employment status; it is not clear whether this meant their present employment status or their employment status at the time of surgery. Type of work was not specified. Patients who were working (full or part time) had a 35% (35/101) risk of pain versus a risk of 14% (14/97) for those who had retired. Thus, the univariable risk difference was 20% (98% CI 8.6–31.8%; our calculation based on table 1 in Poobalan et al, assuming that all patients had the same follow-up time, see above). The comparison was not adjusted for any potential confounders, and duration of post-operative sickness absence was not taken into account. Increasing age was associated with less chronic pain. Risk associated with employment status without any indication of occupational exposures is difficult to interpret, and age probably confounded the comparison. Therefore, the study is hardly informative for the purpose of the present review.
Nienhuijs et al (52) conducted a prognostic study based on a randomized trial that compared three types of open inguinal hernia repair (with mesh). From 2001–2003, 334 patients [97% men (59)] were enrolled in the trial and 96% (N=319) were followed up after a median of 15.4 months. For patients who were employed versus patients who were not employed, the univariable risk difference for persistent pain at follow-up was 12.3% (95% CI 1.4–23.2%; our calculation based on table 2 in Nienhuijs et al, assuming that all patients had the same follow-up time, see above): 48% (90/186) of the employed and 36% (48/133) of the unemployed patients had persistent pain. Duration of post-operative sickness absence was not taken into account. Age was the only predictor that remained significant in a multivariable analysis that also included body mass index, hernia characteristics, surgeon experience, operating time, and type of anaesthesia. With increasing age, less chronic pain was reported, and the majority of the elderly were unemployed. The study did not consider type of employment, and the multivariable analysis suggested that age explained the association between employment and persistent pain.
Berndsen et al (51) reported results of a randomized trial comparing two surgical techniques; Arvidsson et al (50) reported results of the same trial with respect to recurrence, see above. Five years after surgery, 867 (81%) were followed-up with respect to “discomfort”; patients were excluded in case of hernia recurrence. In univariable logistic regression analysis, occupational exposure status was not a prognostic variable for long-term discomfort for either type of surgery; multivariable analyses were not conducted. The result was reassuring, but the considerations listed above regarding Arvidsson et al (50) apply here as well.
Staal et al (54) conducted a prognostic study based on a randomized trial that compared two types of open hernia repair (both with mesh) among patients with a first-time inguinal hernia. From 2004–2005, 172 patients were enrolled, and 88% (of whom 99% were men) were followed for 3 months with respect to pain-related disability as measured by the Pain Disability Index (PDI) that ranges from 0 (best) to 70 (worst). Preoperatively, 41.8% of the patients assessed their employment as light, 29.5% assessed their employment as heavy, and the remaining 28.8% were unemployed or retired. Results showed that light work tended to be associated with a lower PDI preoperatively than heavy work was (12.07 versus 16.65, P=0.06). The difference was statistically significant when assessed 2 weeks after surgery (14.23 versus 20.14, P=0.04), but 3 months after surgery, the difference had disappeared (P=0.57). It was not stated, which proportions had resumed work at these points in time. Results suggested that pain-related disability assessed preoperatively and 14 days post-operatively was more pronounced for patients who rated their work as heavy than for patients who rated their work as light, but the clinical importance of the difference may be limited; this was not discussed. Pain lasting for only 14 days may not qualify as persistent pain. The prospective design was a strength. However, preoperative pain is in general considered a predictor of post-operative pain (30). To the extent that patients with pain overestimated their exposures at the preoperative assessment, information bias may be an explanation of the observed differences.
Gender differences
Men have a constitutional predisposition for both medial and lateral inguinal hernia (cf, the introduction) and women are more likely than men to report prolonged post-operative pain (22, 30). Only two risk studies provided results specifically for women (2, 12). Self-reported physical work activity was not related to inguinal hernia repair in one of these studies (12), whereas in the other, rural residence was a risk factor for first-time inguinal hernia, as a dubious proxy for high physical activity (2). The potential influence of work on post-operative prognosis has almost exclusively been investigated in male study populations.
Discussion
We aimed to make a comprehensive literature search, but we may have missed publications, eg, in languages other than English. We did not include abstracts and unpublished results, and we did not contact authors for original data. However, we find it unlikely that important high-quality studies were overlooked by our search strategy. To be able to retrieve the study (40) that was only identified through a review paper, we revised our search string and succeeded by adding the search term “physical activity”. Using the revised search string, we identified 80 new references, but with the exception of the study that we specifically looked for, none of them fulfilled our criteria for inclusion in the present review. Publication bias was hardly a major problem considering the diverse results. The most important limitation of this review was the poor quality of the reports that we identified regarding risk and prognosis of inguinal hernia in relation to occupational exposures. In particular, the estimated physical efforts or physical (work) activities were indicators of energy expenditure that at the most only indirectly reflected specific occupational risk factors for inguinal hernia or prognostic factors for inguinal hernia repair. Please note that the quality assessment is relative to the focus of the review - some of the reports contained important information with respect to other research questions.
Risk of inguinal hernia by occupation or occupational mechanical exposures
Indications of an increasing risk with increasing physical effort at work were found in one small study that was based on independent exposure assessment but neglected to adjust for confounders (42). Positive associations in three other studies might well be explained by inflationary bias (38, 39, 41), and the negative findings for men in the only prospective study might well be explained by exposure misclassification (2). Two studies reported simple comparisons of cases and controls with respect to average physical work activity, and the average hardly differed between groups (11, 12).
The only prospective study used self-reported crude estimates of physical activity during work (2). The remainder of the studies were based on cross-sectional or retrospective data. The scores used for exposure assessment tended to obscure the nature of the studied exposures even more than would have been the case if job titles had been used per se. None of the studies on occupations or occupational exposures investigated effects of generic occupational exposures such as total daily load lifted, frequency of lifting loads weighing more than a specified number of kilograms, time per day spent standing/walking etc.
In general, outcome assessment was unspecific. First-time and recurrent hernias were often combined so that risk factors and prognostic factors were mixed up. Except for subanalyses in one study (11), none of the studies analyzed lateral and medial hernias separately, and sometimes femoral hernias and even other abdominal hernias were included. The lumping together of different hernia types may have masked relations between exposures and specific outcomes. Among the studies that did not rely on self-reported outcomes, the majority considered hernia repair. Hernia repair may be regarded as a proxy for hernia formation, but since asymptomatic hernias may remain unnoticed, and since asymptomatic and minimally symptomatic hernias may not require surgery, it is impossible to distinguish between risk factors for hernia formation and factors that provoke or aggravate symptoms from a pre-existing hernia in studies focusing on hernia repair. Studies that entail clinical examination [cf. (3)] and maybe ultrasonography of men representing contrasting occupational mechanical exposures could help disentangle these possibilities. However, it may be argued that the distinction is somewhat academic because the heart of the problem is to identify risk factors for symptoms and becoming a patient. When compared to the deficiencies in exposure and outcome assessment, potential lack of blinding of the examiners to exposure status seemed a minor problem.
In the four included case–control studies (11, 12, 41, 42), cases and controls were compared with respect to potential confounders, and non-significant differences were implicitly taken as reassurance that results would not be confounded. This is a fallacy, however, because a potential confounding factor may still be associated with the exposure under study in the population that gave rise to the cases. Only two studies controlled for important potential confounders such as age (2, 3).
Risk of inguinal hernia in relation to a single strenuous event
Effects of single strenuous events were merely studied in case series (43–45). The proportion of hernias that was reported to have a sudden onset varied considerably from study to study, which perhaps reflected the way questions on onset were asked. Case-crossover designs were not employed although these designs have been developed to evaluate if anything unusual took place shortly before the sudden onset of a health outcome (60). Admittedly, a case-crossover study of patients with sudden onset hernias would be an immense challenge, just considering the efforts needed to identify new cases and contact patients shortly after the onset; hernias may even have been present, but unnoticed by the patient before an event that provoked symptoms.
Contributory evidence with respect to risk of hernia formation
Injury mechanisms may involve increased intra-abdominal pressure leading to herniation of the tissues through the inguinal canal or a through a weak point in the abdominal muscles/aponeuroses (http://www.mayoclinic.com/health/inguinal-hernia/DS00364/DSECTION=causes) or the transversalis fascia. Increased intra-abdominal pressure has been hypothesized to be an important stimulus for hernia formation (61). Significant increases in intra-abdominal pressure have been observed during a variety of occupational activities. Among 20 healthy young people, 10 men and 10 women, measured mean pressures while sitting, standing, and walking up a flight of stairs were 17 mmHg, 20 mmHg, and 69 mmHg, respectively, while jumping in place generated the highest pressure of 171 mmHg (62). Intra-abdominal pressure increased with the speed of walking/running up to a mean of 38 mmHg, and intra-abdominal pressures >100 mmHg were often measured in relation to a jump down from a height of 0.4 m (63). A gradual increase in intra-abdominal pressure has been found during sustained lifting, reaching levels around 20 mmHg when the subjects were exhausted after around 8 minutes (64). Intra-abdominal pressures >100 mmHg have been measured during heavy lifting in a stooping position, especially during rapid lifts (65), and intra-abdominal pressures around 120 mmHg have been measured during lifting for a few seconds using maximal force (66). Sudden trunk loading during simulated patient handling situations where the patient fell resulted in peak intra-abdominal pressures of 153 mmHg and 120 mmHg among well-trained men and women, respectively (67). These findings suggest that specific occupational mechanical exposures may be associated with increased intraabdominal pressures and that detailed exposure assessment may be needed in future studies of risk of inguinal hernia in order to reflect this potential injury mechanism.
In childhood, lateral inguinal hernias arise from incomplete obliteration of the processus vaginalis. In a study based on laparoscopy, a patent processus vaginalis was found among 30.9% (29/94) of men and 9.5% (23/243) of women who were on average 50 years old and had not previously undergone inguinal hernia repair (68). During a mean follow-up period of 5.5 years, an inguinal hernia was diagnosed among 11.5% of the patients who had a patent processus vaginalis (at least 4 of these 6 hernias were lateral) and in 3% of the others. The authors concluded that a patent processus vaginalis was a risk factor for lateral inguinal hernias among adults. Although gender stratified (or gender adjusted) analyses would be necessary to reach this conclusion because men have an increased risk of both inguinal hernia and patent processus vaginalis, the study did illustrate that part of the working age male population may be particularly vulnerable to exposures that increase intra-abdominal pressures or otherwise widen the pre-existing opening. Sanjay & Woodward’s (44) observations seem to be consistent with this potential mechanism in that lateral hernias were more likely to have a sudden onset than medial hernias, and a sudden onset was more likely among patients with heavy work. Also in Salcedo-Wasicek & Thirlby’s (53) study, lateral hernias were associated with heavy lifting. Individual vulnerability does not preclude the work-relatedness of disorders that have a multifactorial aetiology, as long as occupational exposures contribute to an increased risk.
Among 53 male athletes (mainly soccer players, mean age 26) with groin pain and no palpable hernia, 4 lateral and 8 medial hernias were diagnosed by X-ray examination after injection of a contrast medium into the peritoneal cavity (69). It was noted that the prevalence of medial hernias was remarkably high, considering the young age of the athletes (69). If corroborated, this observation could generate the hypothesis that peak forces during sports and work may traumatize the transversalis fascia and increase the risk of especially medial herniation. Maybe mechanical exposures can also act through a mechanism involving gradual degradation and weakening of the transversalis fascia (61, 69–71) leading to accelerated age-induced degeneration [cf, the increasing ratio of medial to lateral hernias with age (7)]. In accordance with this, connective tissue alterations have been reported to be more pronounced in patients with a medial inguinal hernia than those with a lateral inguinal hernia (72). Hernia formation has been related to increased elasticity of the transversalis fascia (73) and weak collagen structure and/or defects in collagen (74–76) and elastic fibre (77) metabolism. However, we are not aware of any studies that have related mechanical exposures to pathologic connective tissue alterations in the inguinal region.
Post-operative prognosis by occupation or occupational mechanical exposures
We identified six studies on risk of recurrence after open repair. One older study suggested that medium and heavy work was associated with an increased risk of recurrence (our calculations) (47). Of two underpowered studies, one suggested an increased risk of recurrence in relation to occupational exposures (46) and the other was uninformative (48). Two studies suggested no increase in risk in relation to occupational exposures (49, 50), and one study suggested that early return to work did not increase the risk of recurrence (35). We identified three studies on risk of recurrence after laparoscopic repair; two of these studies indicated an increased risk of recurrence among patients in the exposed groups (40, 49), while the third study did not (50). Across the included studies on recurrence, convalescence tended to increase with occupational exposure intensities, which may have had a protective effect. Convalescence has been shortened considerably since the 1970s without an increasing trend in risk of recurrence. This may in part be explained by increasing use of mesh-based rather than conventional open techniques (78) and in part be related to the fact that the most heavily exposed patients have not shortened their convalescence to the same degree as less exposed patients – they still tend to be on sick leave for 14 days after surgery even when advised to return to work early (35).
Taken together, the studies on post-operative pain in relation to occupational mechanical exposures did not suggest substantial associations, but crude exposure assessment may have masked negative effects of specific exposures, and a protective effect of sick leave may also have obscured any negative impact of occupational exposures on prognosis with respect to persistence of post-operative pain.
Gender differences
Inguinal hernia is primarily a disorder that affects men. The potential influence of occupational mechanical exposures on risk and prognosis has hardly been studied among women.
Comparison with other reviews of the literature and clinical guidelines
A review from 2004 found that the literature did not give a clear answer to the question of whether physical exposures or events are causally associated with hernias, and the review did not find any studies focusing on the association between early return to work and risk of hernia recurrence (34). Four years later, another review stated that activity level seemed to be both protective and detrimental depending on the study in focus, but did not provide references to substantiate the statement (15). A third review, also from 2008, concluded that the sparse literature supported neither a relation between herniation and single or recurrent strenuous events nor a relation between early return to work and reoperation (79). The European Hernia Society has graded the evidence of long-term heavy work as a risk factor for inguinal hernias to level 3 (ie, based on studies of low quality). Thus, our conclusions agree quite well with those of the wider literature. According to the European Hernia Society’s guidelines, heavy weight lifting (probably the sport) should be banned for 2–3 weeks following surgery, whereas other limitations are not warranted (1). Danish clinical guidelines state that patients can be active immediately after surgery when pain is not a hindrance (4). However, prolonged reaction time due to pain has been reported with respect to driving, and this may be the case for operating other machines as well (80).
Degree of evidence for causal and prognostic relations
On the basis of this review, we find that there is insufficient epidemiologic evidence (grade 0) to draw meaningful conclusions about the existence of a causal association between specific occupational mechanical exposures and the development of medial and lateral inguinal hernia. The limited epidemiologic literature, on the other hand, does not rule out important associations, and the contributory evidence with respect to intra-abdominal pressures, a patent processus vaginalis, and – to a lesser extent – connective tissue alterations, points to mechanisms that may link mechanical exposures to inguinal hernia formation.
We also find that there is insufficient epidemiologic evidence (grade 0) to draw meaningful conclusions about the existence of a prognostic association between specific occupational mechanical exposures and negative post-operative outcomes in terms of hernia recurrence and persistent pain. There is no evidence supporting prolonged convalescence in order to avoid recurrence and persistent post-operative pain, but it remains to be shown that patients with high occupational mechanical exposures can safely return to work immediately after surgery.
Research needs
There is a need for high-quality studies of occupational risk factors for lateral and medial inguinal hernia formation in order to corroborate or exclude causal relations. The Danish Hernia Database distinguishes between medial and lateral hernias, which the Danish National Patient Register does not. In collaboration with a researcher from the Danish Hernia Database, three of the authors of this reference document are currently conducting a nationwide male cohort study focusing on quantitative exposure–response relations for medial and lateral inguinal hernias, respectively. Exposure assessment is based on individual job histories according to the Employment Classification Module in Statistics Denmark (81) combined with a JEM based on occupational physicians’ quantitative assessments of generic mechanical exposures (82). The plan is to continue this line of research using data from the Musculoskeletal Research Database at the Danish Ramazzini Centre, which will allow us to take important potential confounders into account (the database contains questionnaire data from around 40 000 persons who have participated in 9 previous studies of musculoskeletal symptoms in the general Danish population or selected occupational groups). Maybe inguinal hernias occur at a younger age in highly exposed jobs, and it would be interesting to explore this hypothesis of risk acceleration (83, 84). The influence of occupational exposures on reoperation rates and prolonged post-operative pain also warrants further study.
Concluding remarks
Inguinal hernia is a common disorder, especially among men, and inguinal hernia repair is one of the most common operations in general surgery. Based on this review, we find that there is insufficient epidemiologic evidence (grade 0) to draw meaningful conclusions about the existence of a causal association between specific occupational mechanical exposures and the development of medial and lateral inguinal hernia. However, contributory evidence points to mechanisms that may link mechanical exposures to inguinal hernia formation. We also find that there is insufficient epidemiologic evidence (grade 0) to draw meaningful conclusions about the existence of a prognostic association between specific occupational mechanical exposures and outcomes after inguinal hernia repair. The limited epidemiologic literature does not rule out important associations. This review revealed several research needs in order to determine if the disorder can be prevented and if the post-operative prognosis can be improved by reducing occupational mechanical exposures.



