The management of work schedules (shift work) has become common in our 24/7 society and increases night work and the diversity of flexible work-hour patterns in industrialized nations (1, 2). Approximately 15% of the fulltime workforce in the United States are shift workers (3). In the European Union (EU), 17% of the workforce are shift workers, while in the EU 27 countries, 19% are night workers (4). In Asia, 22.7% and 15.5% are shiftworkers in Japan (5) and Taiwan (6), respectively. In Korea, shift workers represent 10.9% of the total workforce, and the shift patterns are regular 2 shifts (38.6%), regular 3 shifts (23.9%), 24-hour shift (14.0%), irregular 2 shifts (5.7%), fixed shifts (5.5%), split shifts (3.6%), irregular 3 shifts (2.9%), and “other” (5.8%) (7).
It is well known that several physiological functions follow a circadian rhythm, and long-term disturbance of the circadian rhythm reportedly has clinical consequences. Higher incidences of somatic diseases such as coronary heart disease (8) and metabolic syndrome (9), including obesity and diabetes (10), have been reported among shift workers. Circadian variations in immune defense and inflammation may also be affected by shift effects of occupational exposure. An increase in white blood cell (WBC) count among rotating shift compared to daytime workers has been reported (11, 12). Elevated C-reactive protein was associated with 3-shift work, and 2- and 3-shift work were related with increased WBC count (13).
Periodontal diseases are a group of bacterial inflammatory diseases of the supporting tissues of the teeth. Periodontal disease is one of the most common chronic inflammatory diseases in the world and occurs in at least 35% of the American population (14), 42.5% among Japanese (15), and 33% among Koreans (16). Moreover, periodontitis could be an early sign of severe inflammatory systemic disorder (17).
This study hypothesizes that shift work could be associated with periodontitis, and this association might be mediated by several potential mechanisms including health behaviors (oral health behaviors and other general health behaviors), somatic health problems (obesity and diabetes), and inflammation (measured by WBC count). To the best of our knowledge, there has been no study investigating the association between shift work and oral health. The aim of this study was to examine the relationship between shift work and periodontitis in a large representative sample of an Asian population: the Fourth Korea National Health and Nutritional Examination Survey (KNHANES IV).
Methods
Study population
Data were collected from the 2007–2009 stage of KNHANES IV, a cross-sectional and nationwide survey performed by the Korea Centers for Disease Control and Prevention (KCDC). KNHANES has been performed periodically since 1998 to investigate the health and nutritional status of Koreans. This survey employs a stratified, multi-stage, clustered probability sampling method to select a representative sample of the non-institutionalized, civilian Korean population. The survey is composed of a health interview, a nutrition survey, and a health examination. Oral health has been included as part of the survey since the first year of KNHANES IV. Data were collected by household interviews and direct standardized physical examinations and fasting blood sampling conducted in mobile health examination centers. Each participant in the survey signed an informed consent form. Overall response rates were 65.8% in 2007, 74.3% in 2008, and 79.2% in 2009.
The number of total participants in KNHANES IV was 24 871 (11 310 males and 13 561 females). Among those, periodontal health status was measured for 19 091 participants (8404 males and 10 687 females). Paid workers were 5787 (3089 males and 2698 females) among total participants in KNHANES IV (N=24 871). Exclusion criteria were four-fold: (i) those aged <25 years, (ii) those aged ≥65 years, (iii) the edentate (those with few teeth), and (iv) those missing values in the health assessment or questionnaires. The final sample size for our analysis was 4597 (2528 males and 2069 females (79.4% of all paid workers in KNHANES IV).
Assessment of shift work
Work schedule was derived from the interview question, “Which of the following best describes the hours you usually work at this job?” There were eight possible responses: regular daytime schedule or shift; regular evening shift; regular night shift; rotating 12-hour shift; rotating 24-hour shift; split shift; irregular schedule; or “other”. Shift work was defined as anything but a regular daytime schedule. Of these responses, four broad categories were used to define the type of shift work: evening, night, rotating, and irregular shifts. A rotating shift was defined as a rotating 8-, 12- or 24-hour shift. An irregular shift included split shift, irregular schedule, and “other” (18).
If a respondent asked for clarification of the various shift works at the interview, the following definitions were provided: A regular daytime schedule or shift refers to work beginning after 06:00 and ending before 18:00 hours. A regular evening shift refers to work beginning after 14:00 hours and ending before midnight. A regular night shift refers to work beginning after 21:00 and ending before 08:00 hours. A rotating shift changes periodically from days to evenings or nights. A split shift has two or more distinct periods each day.
Assessment of periodontitis
Dentists conducted an oral health examination in the survey. The World Health Organization (WHO) community periodontal index (CPI) was used to assess periodontitis (19). Periodontitis was defined as a CPI greater than or equal to “code 3”, which indicates that more than one site had a 3.5 mm pocket or larger in the index teeth. The index teeth numbers were 11, 16, 17, 26, 27, 31, 36, 37, 46, and 47, respectively.
Assessment of covariates
Confounders in this study were major sociodemographic factors and included age, gender, income, and education. Mediators considered in the relationship between shift work and periodontitis were oral health behaviors (frequency of daily tooth brushing and regular dental check-up), general health behaviors (smoking and alcohol consumption), somatic health problems (obesity and diabetes), and a measure for inflammation (WBC count). We assumed these mediators as intermediate variables in the causal pathway between shift work and periodontitis. With the exception of obesity, diabetes, and WBC count, information on covariates was collected during the health interview. Education level was categorized into four groups: below primary school, middle school, high school, and college or higher. Monthly household income was adjusted for the number of household members and categorized into four groups: <25, 25–49, 50–75, and >75% of total equalized income in the survey. Information on the frequency of daily tooth brushing was collected from the following question, “How often did you brush your teeth yesterday?” (times/day). Participants were asked whether they had visited a dental clinic for a regular check-up during a year prior to the interview (yes or no). Smoking status was divided into four categories: never smokers, ex-smokers, current smokers who smoked <1 pack per day, and current smokers who smoked ≥1 pack per day. Alcohol consumption was assessed by questioning the participants about their average drinking frequency (days per month or week) during a year prior to the interview. Alcohol consumption status was categorized into five groups: non-drinker, almost non-drinker (≤1 day per month), light drinker (2–4 days per month), moderate drinker (2–3 days per week), and heavy drinker (≥4 days per week). Obesity was measured based on standardized physical examination. Height and weight measurements were performed with the participants wearing light clothing and no shoes. Body mass index (BMI) was grouped as underweight (<18.5 kg/m2), normal (<25 kg/m2) and obese (≥25 kg/m2). Fasting plasma glucose was measured and grouped as normal (<100 mg/dl), pre-diabetic (<126 mg/dl), and diabetic (≥126 mg/dl or diabetic medication). WBC count was measured with blood specimens.
Statistical analysis
Individual sample weights and the complex sample design including stratification and primary sampling units were considered in the analysis.
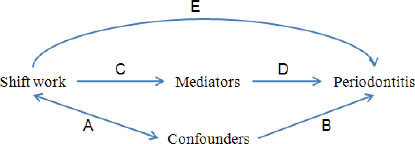
As seen in figure 1, the role of confounders in the relationship between shift work (the independent variable of this study) and periodontitis (the dependent variable of this study) can be determined by examining the association of shift work with confounders (A in figure 1) and the association of confounders with periodontitis (B). Adjusted odds ratio (ORadj) of periodontitis adjusting for sociodemographic variables (age, gender, income, and education) represents the unconfounded total impact of shift work on periodontitis in this study. The relationship of mediators with shift work (C) and periodontitis (D) should also be examined to determine the role of mediators. This role of mediators was evaluated with the percentage (%) excess odd explained, which can be calculated as [(ORadj sociodemographic factors – ORadj sociodemographic factors + mediators) / (ORadj sociodemographic factors – 1)] in this study (20). This % excess odd explained represents the degree to which a mediator explains the relationship between shift work and periodontitis.
Figure 1
A model for the relationship between shift work and periodontitis and the roles of confounders and mediators in the relationship.
In this study, the characteristics of study subjects by periodontitis status were presented with frequency distributions for the categorical variables and means (and standard deviations) for continuous variables (table 1). Chi-square tests for categorical variables and t-tests for continuous variables were used to assess the associations of periodontitis with shift work, confounders, and mediators. Age- and gender-adjusted OR of periodontitis were also presented to show the impact of these covariates on periodontitis. We then presented characteristics of study subjects according to shift work (table 2) and examined the association with Chi-square and t-tests. Series of multiple logistic regression analysis were used to estimate the ORadj of periodontitis according to shift work after adjusting for mediator variables (table 3). The model adjusting for confounders was the base model (model 1 in table 3) in this analysis. Based on these analyses, % excess odd explained were calculated. We also presented findings with full adjustment for shift work and shift patterns (table 4). Due to the ageing difference between shift work and health outcome (21–23), the age-specific subgroup analyses were also performed (table 4).
Table 1
Characteristics of study subjects according to periodontal status: findings from Korea National Health and Nutrition Examination Survey, 2007–2009 (N=4597). Bold denotes statistical significance at P<0.05. [95% CI=95% confidence interval]
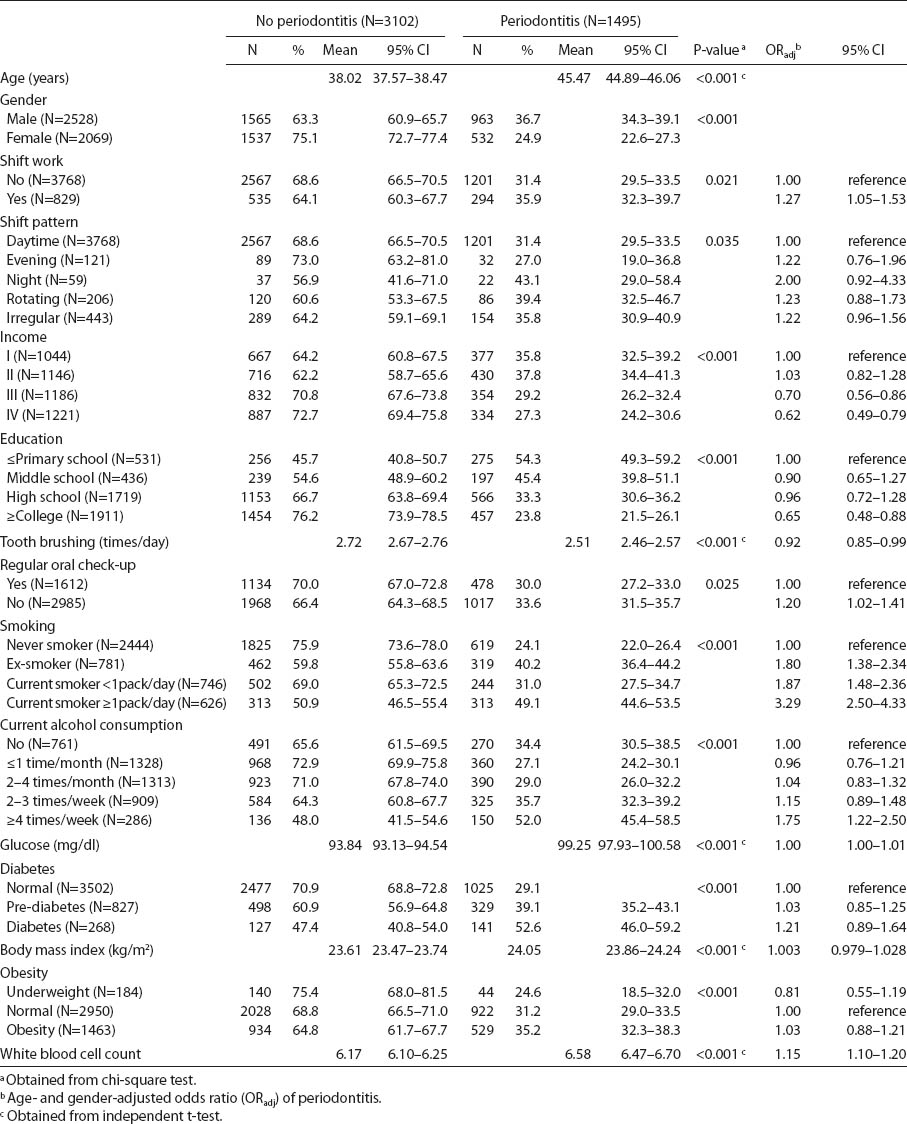
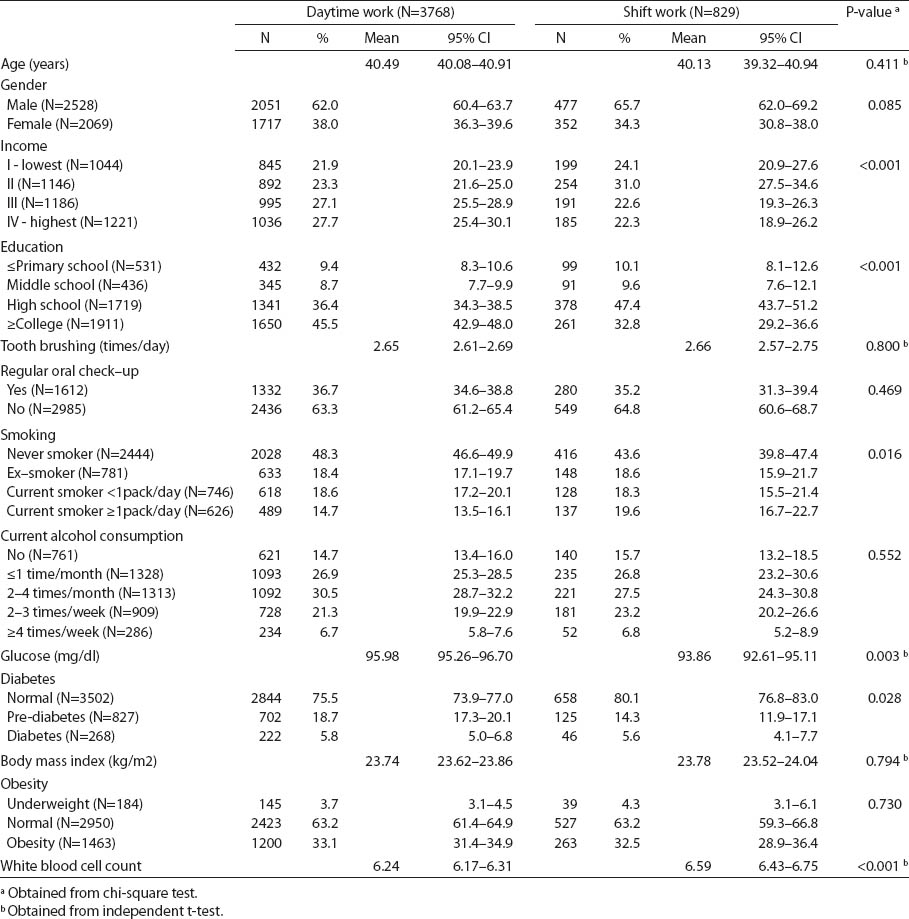
Table 2
Association of shift work and confounders and mediators: Findings from Korea Nation Health and Nutrition Examination Survey, 2007-2009 (N=4597). Bold denotes statistical significance at P<0.05. Bold denotes statistical significance at P<0.05. [95% CI=95% confidence interval]
Results
Of total study subjects (N=4597), 32.3% [95% confidence interval (95% CI) 30.4–34.2%] had periodontitis (CPI ≥3). Table 1 shows that shift workers (N=829) accounted for 18.6% (95% CI 17.1–20.1%) of total study population. According to the shift work patterns, evening shift workers accounted for 2.6% (95% CI 2.1–3.3%), night shift workers 1.3% (95% CI 1.0–1.8%), rotating shift workers 4.5% (95% CI 3.7–5.4%), and irregular shift workers 10.1% (95% CI 8.8–11.6%). Significant differences in the distribution of periodontitis were found with regards to all variables (all P-values <0.05). Except for diabetes, BMI, and obesity, significant age- and gender-adjusted OR of other variables were presented (table 1). Shift work had a significant age- and gender-adjusted OR (ORadj 1.27, 95% CI 1.05–1.53). Night shift showed a relatively great ORadj of 2.00 (95% CI 0.92–4.33) of periodontitis.
Table 2 shows the relationship of shift work with confounders and mediators. Shift work was not patterned by age, gender and frequency of daily tooth brushing (P>0.05). However, shift workers were more likely to have lower income and lower education (all P-values <0.001). There were also significant differences in the distribution of shift work with regards to smoking, blood glucose level, diabetes, and WBC count (table 2).
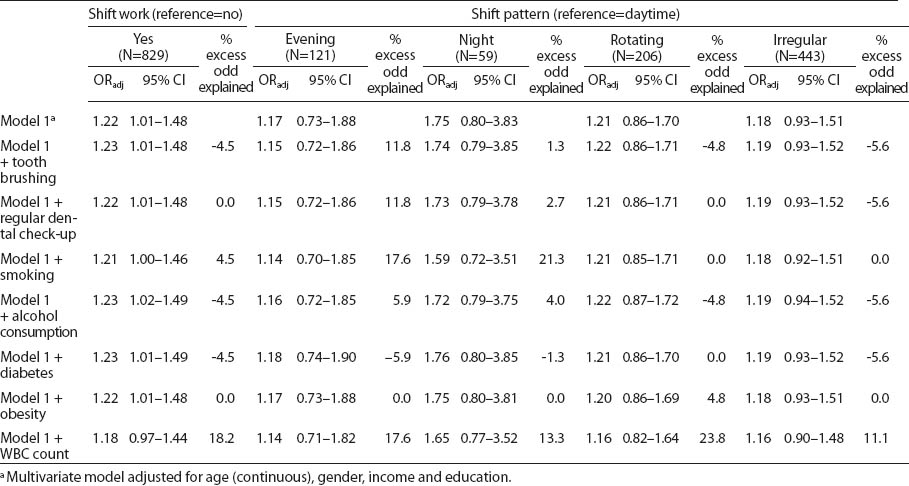
Table 3 shows series of ORadj of periodontitis by shift work and shift work patterns after adjusting for mediators. Model 1 was adjusted for confounders (age, gender, income, and education). The analysis results revealed that shift workers had significantly higher ORadj than daytime workers in the age, gender, income and education-adjusted model (1.22, 95% CI 1.01–1.48). The magnitude of ORadj of periodontitis by shift work attenuated with adjustment for smoking and a marker of inflammation (WBC count). The % excess odd explained was higher for WBC count than others (18.2% versus -4.5% for tooth brushing, 0.0% for regular dental check-up, 4.5% for smoking, -4.5% for alcohol consumption, -4.5% for diabetes, and 0.0% for obesity).
Table 3 also presents the findings by shift pattern. The % excess odd explained was generally higher when WBC count was adjusted in the model. This was true for evening (17.6%), rotating (23.8%), and irregular (11.1%) shift work. In the evening and night shifts, the role of smoking was also important in explaining the relationship between shift pattern and periodontitis. A total of 17.6% (for evening shift) and 21.3% (for night shift) excess odd in the relationship of shift pattern and periodontitis was explained by smoking. Although night shift showed the highest ORadj among the shift work pattern, there was no significant ORadj of periodontitis by shift work pattern.
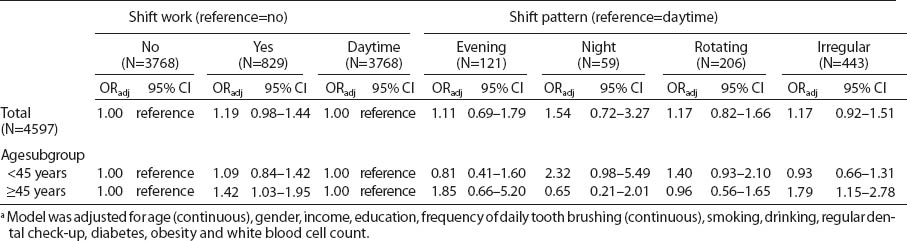
Table 4 shows the ORadj of periodontitis in the fully adjusted model. The magnitude of the relationship between shift work and periodontitis attenuated after controlling for all covariates and was not statistically significant (ORadj 1.19, 95% CI 0.98–1.44).
In the age-specific subgroup analyses (table 4), night shift showed a very high likelihood of having periodontitis among the younger age group (those aged <45 years), although it was not significant. Shift workers aged ≥45 years were more likely to have periodontitis than daytime workers in the same age group (ORadj 1.42, 95% CI 1.03–1.95). Moreover, in this older age group, irregular shift workers showed a significant higher odd of periodontitis than other types of shift workers (ORadj 1.79, 95% CI 1.15–2.78), while night shift did not show any tendency of increased odd of periodontitis.
Discussion
Results of this study identified an epidemiological association between shift work and periodontitis in a representative Korean sample. Analysis results showed that shift workers had a 27% greater odd of having periodontitis than daytime workers in an age- and gender-adjusted model. This association modestly attenuated with further adjustment of socioeconomic status (income and education) but remain statistically significant (ORadj 1.22, 95% CI 1.01–1.48). It is well established that work and the workplace are important social determinants of health (24). Shift work is associated with coronary heart disease (8). Insomnia, a complaint common among night shift workers, is an independent risk factor for myocardial infarction (25). Periodontitis shares common risk factors with metabolic syndrome (26), diabetes mellitus (27), and hypertension (28). Inflammation plays a critical role in the atherosclerotic process (29) and pathogenesis of periodontitis (30). If periodontitis and other systemic diseases could be linked via inflammation, working condition could be considered of risk factors for periodontitis.
In our analysis, we tested the “inflammation” hypothesis with WBC count. Our results showed that WBC count played a role in explaining the relationship between shift work and periodontitis. The % excess odd explained by WBC (18.2%) was higher than the % excess odd explained by other mediators. This was generally true for the relationship between shift pattern and periodontitis. Circadian variations in inflammation may be affected by shift work as WBC count (11–13) increases. Our study suggests that shift work may increase peripheral inflammation measured by WBC count, and WBC count is a relatively independent risk factor.
Smoking showed a dose–response association with periodontitis in our study (table 1), which corroborates a previous finding (31). Moreover, results of this study showed that shift workers were more heavy smokers (current smoker ≥1pack/day) than daytime workers (P=0.016, table 2). Prior studies also presented that shift workers had higher smoking rates than daytime workers (32, 33). In our results, smoking is the second strongest impact on the relationship between shift work and periodontitis and the strongest impact on the relationship between night shift and periodontitis, which supported our hypothesis.
On the other hand, alcohol consumption was not associated with shift work in our study (table 2) and showed negligible % excess odd explained in the relationship between shift work and periodontitis (table 3). Many prior studies could not find differences in alcohol intake between daytime and shift workers (34, 35), although there are some exceptions (32, 36). Time constraints among shift workers might have prevented them from indulging in excessive alcohol consumption, while this would not be the case for smoking. However, detailed mechanisms should be further investigated as to why significant differences in alcohol consumption were not found between daytime and shift workers.
Oral health behavior, frequency of tooth brushing, and regular dental check-up played limited roles in the relationship between shift work and periodontitis in this study. Even though these oral health behaviors predicted the periodontitis (table 1), the differences in these behaviors according to shift work disappeared.
There is considerable epidemiological evidence that shift work is associated with increased risk for obesity and diabetes, perhaps as a result of physiological maladaptation to chronically sleeping and eating at abnormal circadian times. The impact of shift work on metabolism supports a possible pathway to the development of obesity and diabetes (37). However, we could not find an association between shift work and obesity/diabetes and an association between periodontitis and obesity/diabetes.
Our results showed a significant association between shift work and periodontitis among those ≥45 years (ORadj1.44, 95% CI 1.05–1.97). Studies on ageing and shift work show conflicting results. The majority of studies on this topic conclude that tolerance for shift work decreases with age, and that increasing age is associated with increasing negative health effects of shift work (22, 23). The critical age for reduced tolerance to shift and night work is reported to be between 40–50 years (22, 38). The positive association between shift work/irregular shift and periodontitis among the ≥45-year old group might support the above studies. However, night shift work showed the strongest, but non-significant association with periodontitis among the <45-year old group in this study (ORadj 2.34, 95% CI 0.98–5.60). Some have argued that shift work could be better tolerated with older age, and younger people can find it more difficult to adapt to night work due to higher sensitivity to acute sleep loss than older people and because shift work hampers the possibility to participate and integrate in social life (21). Findings indicating that the negative health effects of shift work seem to increase with age might also be explained by factors other than age per se, such as total shift work exposure. Due to the conflicting view on how age is related to shift work tolerance, further studies are needed in different shift work populations and groups with different work schedules.
Although this is the first study to explore the relationship between shift work and periodontitis from the representative national Korean sample, it had some limitations. First, because the duration of shift work was not included in the model, the results of our study, such as the positive association between shift work and periodontitis among ≥45-year-olds, could be biased. The lack of information about the shift work period might be larger among the older than younger workers because the past shift working history was not obtained. Second, irregular shift workers include split shift, irregular schedule, and “other”. Among the respondents in irregular shift workers (N=443), “other”=352. A misclassification bias in using the irregular shift work category could affect both the magnitude and direction of the observed associations of this study. Third, the cross-sectional design prohibited us from inferring causal relationships. Further well-designed prospective investigations are required to determine the causality between shift work and periodontitis to reduce the above-mentioned limitations. Fourth, in addition, the healthy worker effect may have influenced our results. The healthy worker effect states that those who stay in shift work are survivors who can withstand the strenuous shift work and that those who move into daytime work are likely to have a worse health status. Thus, the healthy worker effect may have resulted in an under- rather than overestimation of the effects of shift work.
There is a reason to believe that shift work may become a major occupational oral health and safety problem in the near future. The prevention of shiftwork-related oral health and safety problems will be a major challenge for the employer, employees, and occupational oral health professionals during the next few decades. Our findings have several implications. The increased risk of periodontitis apparent among shift workers suggests that people who do shift work should be vigilant about risk factor modification. Screening programs for periodontal risk factors among shift workers would have yielded substantial help of treatable risks, including dyslipidaemia, hypertension, and cardiovascular diseases. Shift workers should be educated about oral symptoms in an effort to forestall or avert the earliest clinical manifestations of disease. Evidence also exists in the literature to suggest that modification and rationalization of shift schedules may yield dividends in terms of healthier, more productive workers; however, the long-term effects of these alterations on periodontal outcomes remain unknown. There is little evidence for a causal relationship between shift work and periodontitis. To demonstrate causality, we also need studies on mechanisms. We need more prospective studies with large representative populations, good descriptions of the working hours used, long follow-ups, and reliable measurements of health outcomes. More work is needed to identify the most vulnerable subsets of shift workers and the effects of shift modifying strategies on overall oral health.