Febrile seizures are the most common seizure disorder in early childhood, affecting 2–5% of the pediatric population (1). The cause of febrile seizures is unknown, although an attack always involves high fever, with major upper-airway infections, mainly viral, representing the most common provoking factors (2–4).
Air pollution and road traffic noise are common environmental exposures, which co-exist because road traffic is a major source of both. Studies have found associations between outdoor air pollution and higher risk of ear infections and respiratory infections among children, including viral infections and influenza-like illness (5–9). It is believed that air pollution induces oxidative stress, increases inflammatory responses, and reduces the ability of macrophages to phagocytize or inactivate viruses (10–14). Due the immaturity of their immune system, children are considered to be especially vulnerable to the effects of air pollution (15).
Traffic noise is thought to be hazardous through activation of a general stress response and disturbance of nighttime sleep (16). Although research has focused on adults, some studies have suggested that exposure to aircraft and road traffic noise increase levels of catecholamine and cortisol secretion among children (17, 18). Exposure to traffic noise has also been associated with sleeping problems in children (18, 19). For example, a German study of 10-year-old children reported that nighttime road traffic noise at the least exposed façade (quiet side) was significantly associated with problems falling asleep as well as “any sleeping problems” (19). Studies among humans as well as animals have found that stress and disturbance of sleep affects the immune system negatively, which may lead to increased susceptibility to viral infections (20–23). Also, a few recent animal and human studies have found associations between traffic-noise exposure and the immune system, including an effect on the level of natural killer cells, which is a critical part of the innate immune system and known to respond rapidly to cells infected with virus (24, 25). In addition, an animal study has indicated that exposure to prenatal stress enhances the development of febrile seizures in rats (26). The suspected mechanisms include activation of the hypothalamic-pituitary-adrenal axis, leading to elevated concentrations of glucocorticoids, which have been shown to be toxic to those regions of the nervous system that are easily excitable, such as the pyramidal cells of the hippocampus (26).
Using data from a large population based cohort, this study aimed to investigate whether residential exposure to road traffic noise and air pollution during early life are associated with risk for febrile seizures in childhood.
Methods
Study population
The study was based on children enrolled in the Danish National Birth Cohort (DNBC) (27), which consecutively recruited pregnant women from March 1996 to November 2002 from all over Denmark. Women who spoke Danish and intended to carry their pregnancy to term were invited to participate in the cohort at the first pregnancy consultation with their general practitioner. After providing written informed consent, the women participated in two computer-assisted telephone interviews, conducted by trained interviewers around mean gestational weeks 16 and 31, including questions on smoking habits, alcohol consumption, and parity. When the child was seven, a follow-up questionnaire was mailed to the parents. In total, parents of 57 282 children participated. For these children, we gained information on childhood addresses and traffic exposures for use in studies based on outcome information obtained in the seven-year questionnaire (28, 29). These 57 282 children, therefore, constituted the study base of the present study (for the DNBC children not participating in the seven-year questionnaire, we did not have address or exposure information during childhood). The DNBC was established following the Danish Scientific Ethics Committee approval (case number (KF) 01-471/94) and the Danish Data Protection Agency approved all data collections.
Outcome
Children with febrile seizures were identified by linking the unique personal identification number of each child in the study base to the nationwide Danish National Patient Register (DNPR), in which diagnostic codes are collected for all persons treated as out- or inpatients at all Danish hospitals (30). These diagnostic codes are based on the International Classification of Diseases, 10th revision (ICD10) from 1994 and onward. Children were identified as cases if they were registered with the ICD10 code R56 in the period between three months and five years of age (until the day before their sixth birthday) as febrile seizures occurs within this age span (1). Children with a diagnosis of epilepsy (ICD10 codes: G40–G41) before a diagnosis of febrile seizures were not included as cases. We only included the first diagnosis of febrile seizures.
Exposures
Residential address history for all children participating in the seven-year follow-up questionnaire (N=57 282) between conception and end of follow-up (event, death, emigration or five years of age) were collected from the Danish Civil Registration System. All addresses were geocoded.
We estimated annual levels of road traffic and railway noise at all addresses using SoundPLAN; a calculation program based on the Nordic prediction method. The Nordic prediction method has been a standard method for noise calculation in Scandinavia during many years (31). A validation of the method based on a number of measurements in up to 300 m from the road, found the average difference between measurements and calculations to be 0.2 dB, showing that the model is very accurate (31, 32). The noise model requires information on geocode and height for each address and polygons (in 3D) for all buildings in Denmark. Furthermore, traffic input variables for estimation of road traffic noise were annual average daily traffic and distribution of light and heavy vehicles for all Danish road links, as well as travel speed and road type for all road links (motorway, express road, road wider than 6 m, road narrower than 6 m and wider than 3 m, and other road). All information on traffic was obtained from a national road and traffic database, which contains information for roads with >1000 daily vehicles (33). For estimation of railway noise, traffic input variables were annual average daily train lengths, train types, travel speed (obtained from Banedanmark, which is operating the Danish state railway network). For both road traffic and railway noise modelling, we assumed that the terrain was flat and that roads, urban areas and areas with water were hard surfaces, and that all other areas were acoustically porous. We included information on railway noise barriers, but did not have information on road surface and road noise barriers. We calculated road traffic and railway noise as the equivalent continuous A-weighted sound pressure levels at the most exposed facade of each residence during day, evening and night, and expressed noise exposure as Lden (34).
We used the Danish AirGIS dispersion modelling system (envs.au.dk/videnudveksling/luft/model/airgis/) to calculate exposure to trimester-specific NO2 levels at all pregnancy addresses as well as annual levels of NO2 for all childhood addresses (35). AirGIS calculates air pollution as hourly time series at each address as the sum of: (i) air pollution from the nearest street, calculated using information on traffic (intensity, type, speed; same as described for noise), geometry of buildings and streets (street canyons), car fleet emission factors, and meteorology; (ii) urban background, and (iii) regional background, estimated from rural monitoring data and national vehicle emissions. Urban background concentration is calculated in a 1×1 km resolution taking into account emissions from all sectors, city dimensions and building heights including historic trends, while the local street contribution is calculated at the building façade near the closest and most trafficked road with a few meters resolution. Several studies have successfully validated and applied air pollution estimates modelled by AirGIS (36–39). Regarding validation, the correlation between modeled and measured mean half-year NO2 concentrations at 204 positions in Greater Copenhagen conducted in the period 1994–1995 was found to be 0.90 (36). Also, the correlation between modeled and measured 1-month mean concentrations of NO2 in a busy street in Copenhagen during 1995–2006 was found to be 0.67 (37). NO2 serves as proxy for the mix of traffic-related air pollutants.
Statistical analysis
Analyses were based on Cox proportional hazard models, using age as the underlying time. We used left truncation at three months of age, such that the children were considered at risk from that age, and right censoring at the age of febrile seizure (event), death, emigration or until the day before they reached six years of age, whichever occurred first. We analyzed two exposure windows: pregnancy and childhood. Exposure to road traffic noise and air pollution during pregnancy was modelled as mean exposure, taking all addresses during pregnancy into account. Childhood exposures were modelled as the yearly mean exposure at the diagnosis address and entered as time-dependent variables into the statistical risk model, thus, for each case of febrile seizure comparing with exposure for all cohort participants at exactly the same age as the case at the time of diagnosis.
Incidence rate ratios (IRR) for febrile seizure per interquartile range (IQR) increase in exposure to road traffic noise and air pollution were analyzed in three models: model 1 with adjustment for age (by design); model 2 with further adjustment for the following a priori defined confounders (40): sex of the child, maternal age at birth (years, linear) (obtained from the Danish Medical Birth Registry), parity (0, 1, ≥ 2), smoking during 1st trimester (no, yes), alcohol consumption during first trimester (no; yes, <1 drink/week; yes, ≥1 drink/week), level of education [highest attained education at birth of the child: basic (7–12 years of primary, secondary and grammar-school education), vocational (10–12 years of education) and higher (≥13 years of education)], disposable income one year before birth of the child (quintiles, household income after taxation and interest per person, adjusted for number of persons in the household and deflated according to the year 2000 value of the Danish krone). In model 3, we adjusted road traffic noise for air pollution and vice versa, (for same exposure time-windows). We also generated five quintiles of exposure to road traffic noise/air pollution among cases at the time of diagnosis, and estimated IRR (model 2) of the four higher categories as compared with the lowest category (reference). All information on socioeconomic position (SEP) was obtained from the national register Statistic Denmark.
Linearity of continuous variables (road traffic noise, air pollution and maternal age) were investigated by graphical evaluation using linear spline models with boundaries at deciles among cases. No deviation from linearity was found. The proportional hazards assumption was tested by graphical inspection, and revealed no deviation from the assumption.
We estimated the association between road traffic noise/air pollution and febrile seizure cases in predefined sub-groups by sex, gestational age (< and > 37 weeks), maternal education at time of birth (basic, vocational and high), maternal smoking during 1st trimester (from 1st pregnancy interview) and parity (nulliparous, uniparous and multiparous). Potential effect modification was evaluated by introducing an interaction term into the model and tested by Wald test.
We conducted a sensitivity analysis, where we excluded children, whose mothers already participated in the study population with one child. All analyses were performed using SAS version 9.3 (SAS Institute, Cary, NC, USA).
Results
Of the 57 282 children participating in the seven-year follow-up questionnaire, we excluded 2374 who were not singletons, 949 with missing exposure information, 2494 with missing information on one or more potential confounders, leaving a study population of 51 465 children of whom 2175 were diagnosed with febrile seizures during the follow-up period.
Children with febrile seizures were more likely to be boys and the first-born child, whereas only small differences were seen between the cases and the cohort with regard to maternal age, maternal education, household disposable income, maternal smoking and maternal alcohol consumption (table 1). Residential exposure to air pollution and road traffic noise were correlated; eg, the pregnancy exposures were positively correlated with r-Spearman=0.47. Also, exposures during pregnancy and childhood were correlated; the Spearman correlations were 0.49 for road traffic noise and 0.38 for air pollution. The distributions of exposure to road traffic noise and air pollution (during pregnancy) are shown in supplementary figure 1 (www.sjweh.fi/show_abstract.php?abstract_id=3724).
Table 1
Characteristics of the study population by febrile seizure status
| Total population (N=51 465) | Febrile seizure cases (N=2175) | |
|---|---|---|
|
|
|
|
| % Median (5–95 percentiles) | % Median (5–95 percentiles) | |
| Maternal age at conception (years) | 30.4 (24.0–37.9) | 30.1 (23.8–37.8) |
| Sex | ||
| Boys | 51 | 54 |
| Girls | 49 | 46 |
| Parity | ||
| Nulliparous | 47 | 53 |
| Uniparous | 37 | 34 |
| Multiparous | 16 | 14 |
| Mother’s highest educationa | ||
| Basic (7–12 years) | 11 | 12 |
| Vocational (10–12 years) | 47 | 45 |
| Higher (≥13 years) | 42 | 43 |
| Disposable income (quintiles)b | ||
| Q1 (low) | 10 | 10 |
| Q2 | 11 | 12 |
| Q3 | 22 | 20 |
| Q4 | 30 | 19 |
| Q5 (high) | 27 | 29 |
| Maternal smokingc | ||
| No | 86 | 84 |
| Yes | 14 | 16 |
| Maternal alcohol consumptionc | ||
| No alcohol | 75 | 76 |
| <1 drink/week | 13 | 14 |
| >1 drink/week | 11 | 11 |
| Exposures | ||
| Road traffic noise (dB)d | 57.5 (49.4–69.6) | 57.9 (49.9–69.5) |
| Air pollution (NO2, µg/m3)d | 10.9 (7.1–26.1) | 11.0 (7.1–26.5) |
| Railway noise, Lden > 40 dB | 12 | 14 |
Figure 1
Associations between residential childhood exposure to road traffic noise (A) and air pollution (B) and risk of febrile seizures adjusted for sex, maternal age, socio-economic position, parity, maternal lifestyle factors, and calendar-year. The vertical whiskers show incidence rate ratios with 95% confidence interval at the median of the exposure categories (quintiles) compared with the reference category.
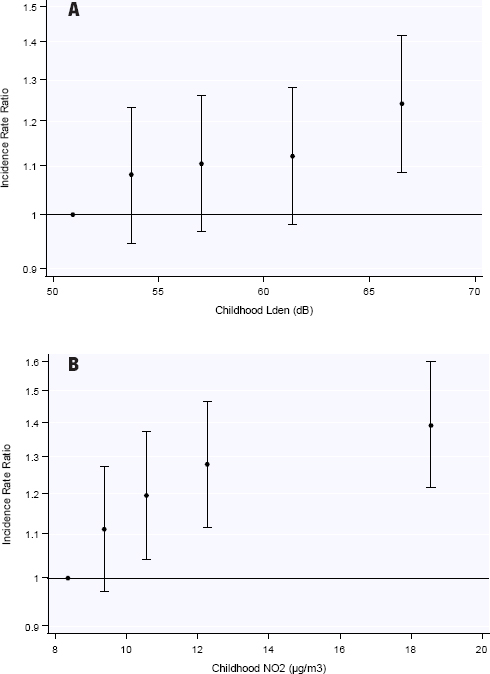
Associations between an IQR increase in exposure to road traffic noise and air pollution and risk for febrile seizure are shown in table 2 (associations per 10 unit increase are shown in supplementary table A, www.sjweh.fi/show_abstract.php?abstract_id=3724). In the crude analyses, exposure to road traffic noise and air pollution during both exposure time windows was associated with a statistically significant increase in risk. In adjusted analyses (model 2), exposure to childhood road traffic noise and air pollution was statistically significant associated with a higher risk for febrile seizures: an IQR increase in exposure to road traffic noise and air pollution was associated with an 11% (95% CI 1.04–1.19) and 5% (95% CI 1.02–1.07) higher risk for febrile seizures, respectively. The associations appeared to follow a monotonic exposure–response relationship for both exposures (figure 1). The same tendencies were seen for pregnancy exposure, but the estimates were statistically insignificant. In two-pollutant models with mutual exposure adjustment, the estimates were lower, but there was still a statistically significant association with childhood exposure to road traffic noise (IRR 1.08, 95% CI 1.00–1.16) and an insignificant association for air pollution (IRR 1.03, 0.99–1.06). We found no associations between exposure to railway noise and risk for febrile seizures (supplementary table B, (www.sjweh.fi/show_abstract.php?abstract_id=3724).
Table 2
Associations between residential exposure (linear) to road traffic noise and air pollution during pregnancy and at diagnosis and risk for incident febrile seizures among 51 465 children. [IRR=incidence rate ratio; CI=confidence interval; IQR=interquartile range]
| Exposures | Model 1a IRR (95% CI) | Model 2b IRR (95% CI) | Model 3c IRR (95% CI) |
|---|---|---|---|
| Mean exposure during pregnancy | |||
| Road traffic noise (Lden, per IQR: 9.5 dB) | 1.09 (1.02–1.16) | 1.06 (0.99–1.13) | 1.06 (0.98–1.14) |
| Air pollution (NO2, per IQR: 5.5 µg/m3) | 1.03 (0.99–1.06) | 1.02 (0.98–1.06) | 1.00 (0.96–1.05) |
| Yearly exposure at diagnosis address | |||
| Road traffic noise (Lden, per IQR: 9.5 dB) | 1.13 (1.06–1.21) | 1.11 (1.04–1.19) | 1.08 (1.00–1.16) |
| Air pollution (NO2, per IQR: 4.0 µg/m3) | 1.06 (1.03–1.09) | 1.05 (1.02–1.07) | 1.03 (0.99–1.06) |
We found that the associations between both exposures and risk for febrile seizures were significantly modified by parity, with higher estimates among children with older siblings, compared to children born as the first child (table 3). No other significant effect modifications were found.
Table 3
Modification of associations between yearly road traffic noise and air pollution [per interquartile range (IQR) Lden 9.5 dB; NO2 4.0 µg/m3] at the residential address at time of diagnosis and risk for febrile seizures by sex, gestational age, education, smoking and parity. [IRR=incidence rate ratio; CI=confidence interval]
| Covariates | N cases | Road traffic noise (per IQR) | Air pollution (NO2 per IQR) | ||
|---|---|---|---|---|---|
|
|
|
||||
| IRR (95% CI)a | Pinteraction | IRR (95% CI)a | Pinteraction | ||
| Sex | 0.60 | 0.76 | |||
| Boys | 1179 | 1.10 (1.01–1.19) | 1.05 (1.01–1.09) | ||
| Girls | 996 | 1.13 (1.03–1.25) | 1.04 (1.00–1.08) | ||
| Gestational age | 0.59 | 0.60 | |||
| <37 weeks | 150 | 1.04 (0.82–1.33) | 1.07 (0.97–1.18) | ||
| ≥37 weeks | 2025 | 1.12 (1.05–1.19) | 1.04 (1.02–1.07) | ||
| Maternal education (years) | 0.90 | 0.99 | |||
| Basic (7–12) | 263 | 1.15 (0.96–1.38) | 1.04 (0.95–1.14) | ||
| Vocational (10–12) | 976 | 1.10 (1.00–1.21) | 1.05 (1.00–1.09) | ||
| Higher (≥13) | 936 | 1.12 (1.01–1.23) | 1.05 (1.01–1.09) | ||
| Maternal smoking | 0.56 | 0.62 | |||
| No | 1828 | 1.16 (0.99–1.35) | 1.03 (0.96–1.11) | ||
| Yes | 347 | 1.10 (1.03–1.18) | 1.05 (1.02–1.08) | ||
| Parity | 0.01 | 0.01 | |||
| Nulliparous | 1146 | 1.02 (0.93–1.11) | 1.02 (0.98–1.05) | ||
| Uniparous | 734 | 1.23 (1.11–1.38) | 1.09 (1.04–1.15) | ||
| Multiparous | 295 | 1.25 (1.04–1.49) | 1.14 (1.04–1.26) | ||
In a sensitivity analysis, we excluded the 2788 children, whose mothers already participated in the study population with one child. This resulted in only minor changes in estimates: for model 2 the IRR for childhood road traffic noise was 1.11 (95% CI 1.04–1.19) and for air pollution the IRR was 1.04 (95% CI 1.01–1.07).
Discussion
The present study indicated that residential exposure to road traffic noise and air pollution during childhood are associated with a slightly higher risk for febrile seizures, following a monotonic exposure–response relationship. In analyses with mutual exposure adjustment, the estimates were lowered, but they still reached statistical significance for childhood exposure to road traffic noise and borderline significant for childhood exposure to air pollution. For both exposures, higher estimates were observed among children with older siblings compared to children born as first child. Pregnancy exposure to the two pollutants also seemed associated with febrile seizures, though estimates were weaker and statistically non-significant.
We have not been able to identify other studies investigating the association between exposure to road traffic noise and air pollution and risk for febrile seizures, and also studies on the mechanisms of traffic noise in children are rare. Therefore, results should be interpreted with caution. However, our finding of positive associations with risk for febrile seizures are supported by a number of studies showing that exposure to air pollution is associated with upper airway and ear infections, which are the most common provoking factors for febrile seizures (5–9). Similarly, studies have found that both stress and disturbance of sleep, which are the believed mechanisms behind an association between traffic noise and disease (16), may increase susceptibility to viral infections (20–23). In addition, studies in animals and humans have found associations between traffic noise and the immune system, including an effect on natural killer cells, known to respond rapidly to viral infections (24, 25). However, the association between noise exposure and the immune system has only been investigated in vanishing few studies, and more research are needed. Our findings are, furthermore, supported by the observed monotonic exposure–response relationships. It therefore seems possible that air pollution and road traffic noise may affect the immune system, thereby increasing risk for viral infections, which again may increase the risk for febrile seizures.
In the present study, road traffic noise and air pollution were correlated, which reflects that road traffic is a source of both exposures. However, the correlation is moderate with an R2 of 0.22 for the pregnancy exposure, and thus 78% unexplained variation. In analyses with mutual exposure adjustment, the estimates for both road traffic noise and air pollution were slightly lowered, indicating a small mutual confounding. However, the estimates were still statistically significant for childhood exposure to road traffic noise and borderline significant for childhood exposure to air pollution, indicating that both of these co-existing traffic pollutants affects the risk for febrile seizures. We cannot rule out that the exposure models predicts road traffic noise more precisely than air pollution, which could potentially explain the apparent more robust association with road traffic noise.
Interestingly, we found higher risk estimates among children with older siblings compared to children born as first child. It is well-known that having (older) siblings, are associated with a higher risk for infections, as siblings represent possible carriers of infections acquired in kindergartens and schools, where many children spend time together indoors, which increases the risk for spreading of infections (41). Our finding may indicate that for traffic noise and air pollution to increase the risk for developing febrile seizures, the child needs to be in contact with a certain level of exposure to viral agents.
When investigating pregnancy exposure to noise and air pollution we found weaker and statistically insignificant associations, which indicates that prenatal exposure to these traffic pollutants are not important in relation to development of febrile seizures.
Our study has several strengths including its size, access to residential address histories from conception until censoring, and information on various potential confounders obtained from nationwide registers and questionnaires (questionnaire information on confounders were collected before birth of the child, and thus with no risk of recall bias). Furthermore, information on the outcome was obtained from a high-quality hospital registry (30). A validation study found that registration of febrile seizures in the DNPR were generally good, with a completeness of 72% and a predictive value of 93% (42). Road traffic noise and air pollution were estimated using good input data and state-of-the art exposure models.
However, some limitations have to be considered. The estimation of noise and air pollution was based on modeled values, and although both the Nordic prediction method and the AirGIS model have been used for many years, estimation of these exposures will be associated with some degree of uncertainty. We had no information on various individual factors that might influence personal exposure to noise or air pollution, such as information on time spent at home, window opening habits, workplace and kindergarten addresses, and the preferred mode and duration of commuting to work or kindergarten. This may have resulted in exposure misclassification. However, we would expect such misclassification to be unrelated to febrile seizures, and therefore most likely influence the relative risk estimate towards the neutral value. Furthermore, we identified only cases with febrile seizures based on hospital admissions and/or outpatient visits, and might, thus, have overlooked those, who did not seek treatment. However, febrile seizures are a frightening experience for most parents, and, in Denmark, general practitioners are encouraged to admit children with a first episode of febrile seizures for further investigation in hospitals. Although adjustment for the confounders included in the present study resulted only in minor changes in IRR, we cannot rule out residual confounding from eg, socioeconomic factors or confounding by factors not adjusted for, such as population density and crowding in the home or in kindergarten. Studies have suggested that although house prices are known to be negatively associated with traffic exposures, the relationship between traffic exposure and socioeconomic position may not always be pronounced, as living in city centers of large metropolitans are popular, attracting residents of high socioeconomic position (43). Similarly, we observed in the present study that the difference in the traffic exposures between women with high versus basic education was small, with mean levels of 11.5 and 11.2 µg/m3 for NO2, respectively, and 57.0 dB and 57.6 dB for road traffic noise, respectively.
Our study population was based on children participating in the seven-year follow-up questionnaire because we had gained address and exposure information during childhood for this population. This might have introduced selection bias. However, the presence and magnitude of bias was not possible to assess. Lastly, only around 30% of all eligible pregnant women participated in the DNBC. A previous study indicated that women of low socioeconomic position (measured by education, occupation, income and marital status) might be underrepresented in the cohort (44). Although this hampers the generalizability of the present study, an evaluation study of bias induced by non-participation found only small differences on selected associations between the DNBC cohort and the general population.
In conclusion, the present study indicates that exposure to residential road traffic noise and air pollution may be associated with higher risk for febrile seizures. However, as this is the first study of its kind, further studies are needed to confirm or reject the results.



